Essay on Smoking
500 words essay on smoking.
One of the most common problems we are facing in today’s world which is killing people is smoking. A lot of people pick up this habit because of stress , personal issues and more. In fact, some even begin showing it off. When someone smokes a cigarette, they not only hurt themselves but everyone around them. It has many ill-effects on the human body which we will go through in the essay on smoking.


Ill-Effects of Smoking
Tobacco can have a disastrous impact on our health. Nonetheless, people consume it daily for a long period of time till it’s too late. Nearly one billion people in the whole world smoke. It is a shocking figure as that 1 billion puts millions of people at risk along with themselves.
Cigarettes have a major impact on the lungs. Around a third of all cancer cases happen due to smoking. For instance, it can affect breathing and causes shortness of breath and coughing. Further, it also increases the risk of respiratory tract infection which ultimately reduces the quality of life.
In addition to these serious health consequences, smoking impacts the well-being of a person as well. It alters the sense of smell and taste. Further, it also reduces the ability to perform physical exercises.
It also hampers your physical appearances like giving yellow teeth and aged skin. You also get a greater risk of depression or anxiety . Smoking also affects our relationship with our family, friends and colleagues.
Most importantly, it is also an expensive habit. In other words, it entails heavy financial costs. Even though some people don’t have money to get by, they waste it on cigarettes because of their addiction.
How to Quit Smoking?
There are many ways through which one can quit smoking. The first one is preparing for the day when you will quit. It is not easy to quit a habit abruptly, so set a date to give yourself time to prepare mentally.
Further, you can also use NRTs for your nicotine dependence. They can reduce your craving and withdrawal symptoms. NRTs like skin patches, chewing gums, lozenges, nasal spray and inhalers can help greatly.
Moreover, you can also consider non-nicotine medications. They require a prescription so it is essential to talk to your doctor to get access to it. Most importantly, seek behavioural support. To tackle your dependence on nicotine, it is essential to get counselling services, self-materials or more to get through this phase.
One can also try alternative therapies if they want to try them. There is no harm in trying as long as you are determined to quit smoking. For instance, filters, smoking deterrents, e-cigarettes, acupuncture, cold laser therapy, yoga and more can work for some people.
Always remember that you cannot quit smoking instantly as it will be bad for you as well. Try cutting down on it and then slowly and steadily give it up altogether.
Get the huge list of more than 500 Essay Topics and Ideas
Conclusion of the Essay on Smoking
Thus, if anyone is a slave to cigarettes, it is essential for them to understand that it is never too late to stop smoking. With the help and a good action plan, anyone can quit it for good. Moreover, the benefits will be evident within a few days of quitting.
FAQ of Essay on Smoking
Question 1: What are the effects of smoking?
Answer 1: Smoking has major effects like cancer, heart disease, stroke, lung diseases, diabetes, and more. It also increases the risk for tuberculosis, certain eye diseases, and problems with the immune system .
Question 2: Why should we avoid smoking?
Answer 2: We must avoid smoking as it can lengthen your life expectancy. Moreover, by not smoking, you decrease your risk of disease which includes lung cancer, throat cancer, heart disease, high blood pressure, and more.
Customize your course in 30 seconds
Which class are you in.

- Travelling Essay
- Picnic Essay
- Our Country Essay
- My Parents Essay
- Essay on Favourite Personality
- Essay on Memorable Day of My Life
- Essay on Knowledge is Power
- Essay on Gurpurab
- Essay on My Favourite Season
- Essay on Types of Sports
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Download the App


Essay on Teenage Smoking
Students are often asked to write an essay on Teenage Smoking in their schools and colleges. And if you’re also looking for the same, we have created 100-word, 250-word, and 500-word essays on the topic.
Let’s take a look…
100 Words Essay on Teenage Smoking
What is teenage smoking.
Teenage smoking means when young people, usually between 13 and 19 years old, start to smoke cigarettes. It is a big problem because it can harm their health very badly. Smoking can cause diseases like cancer and heart problems.
Why Do Teenagers Start Smoking?
Many teenagers start smoking because they see their friends doing it or they think it makes them look cool. Sometimes, they are under a lot of stress and think smoking will help them relax.
Effects of Smoking on Teenagers
Smoking can make teenagers sick. It can reduce their lung function and make it hard for them to breathe. It also increases the risk of getting sick with diseases like bronchitis and pneumonia.
Stopping Teenage Smoking
To stop teenagers from smoking, adults should talk to them about the dangers of smoking. Schools can also help by teaching students about the risks of smoking and how to say no to cigarettes.
250 Words Essay on Teenage Smoking
One main reason teenagers start smoking is peer pressure. They see their friends doing it and don’t want to feel left out. Some teenagers think smoking makes them look cool or grown-up. Others might start smoking because they are curious or because they see family members smoking.
Smoking is very harmful to anyone’s health, but it is especially bad for teenagers because their bodies are still growing. Smoking can lead to serious health problems like lung cancer, heart disease, and breathing problems. It also affects how they look, causing bad breath, yellow teeth, and a greater risk of getting sick.
Stopping teenage smoking is important. Parents, teachers, and communities can help by teaching teenagers about the dangers of smoking. They can also set a good example by not smoking themselves. Programs that encourage teenagers to stay away from cigarettes and offer support to those who want to quit are also very helpful.
In conclusion, teenage smoking is a problem that affects the health and future of young people. By understanding why teenagers start smoking and the effects it has, we can work together to help stop it.
500 Words Essay on Teenage Smoking
Teenage smoking: a grave threat to young lives.
Smoking among teenagers has become a pressing concern, posing significant risks to their health and overall well-being. It’s crucial to understand the harmful effects of smoking and take proactive measures to prevent and discourage teenagers from engaging in this dangerous habit.
Health Hazards of Teenage Smoking
Negative impact on physical development.
Smoking interferes with the normal growth and development of teenagers. It can stunt their physical growth, delay puberty, and weaken their immune system, making them more susceptible to illnesses. Smoking also affects bone health, increasing the risk of osteoporosis in later life.
Social and Psychological Effects
Teenage smoking has detrimental social and psychological consequences. It can lead to isolation, peer pressure, and impaired social skills. Smokers are more likely to engage in risky behaviors, such as alcohol consumption and drug abuse. Moreover, smoking can negatively impact academic performance, concentration, and memory.
Preventing Teenage Smoking
Teenage smoking is a serious public health issue that demands immediate attention. It’s essential to raise awareness about the harmful effects of smoking and empower teenagers with the knowledge and skills to resist tobacco use. By working together, we can create a smoke-free environment for our youth, ensuring their health and well-being for a brighter future.
That’s it! I hope the essay helped you.
Happy studying!
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *

Academia.edu no longer supports Internet Explorer.
To browse Academia.edu and the wider internet faster and more securely, please take a few seconds to upgrade your browser .
Enter the email address you signed up with and we'll email you a reset link.
- We're Hiring!
- Help Center

Essay: Causes and Effects of Smoking Among Students

Smoking is one of the most dangerous widespread phenomena that threaten lives of a huge number of people worldwide. It starts as a way of having fun, but ends as an addiction that is therefore so difficult to give up. Today, we often hear of “smoking among students”. So why do students smoke and what are the effects that smoking has on them?
Related Papers
The Journal of Contemporary Issues in Business and Government
Tabssum Naz
Introduction: The World Health Organisation has declared that smoking is the biggest health problem, since over four million people die because of it every year and it causes much harm. The assumption that all over the world, including Turkey, about 45% of the population over 15 years old has a smoking habit on a very serious scale reveals how important the problem is for the young population. Material and Method: This study was carried out to determine the smoking status of the final grade students at Atatürk University in the 2003-2004 academic year. A questionnaire form developed by the researchers was used as the data gathering tool. Results: It was found that 42.0% of the participants had smoked (continuous and occasional smoking). The age of onset of smoking was mainly between 14 and 21 years. There was a statistically strong association between duration of smoking, starting time, and smoking amount (p<0.001), including the association between age of onset and smoking status of the students (p<0.05). Of the students, 22.1% stated that they did not know why they started smoking. Their main answers were; 56.5% of them stated they smoked to relieve their stress feelings, 24.6% stated they smoked for pleasure. Conclusion: Cigarette are widely used by university students. The reason why the students started smoking was mostly fellowship environment, and the reason for continuing to smoke was mostly to relieve stress. (Tur Toraks Der 2008;9:93-8) Key words: Smoking, university student, Erzurum, Turkey.
Journal of emerging technologies and innovative research
Dr. Manjur Hossain
IJHASS Journal
International Journal of Public Health Science (IJPHS)
Smoking is the main cause of morbidity and mortality in the world and is estimated to kill 5 million people each year worldwide. If current patterns of tobacco consumption continue, smoking will kill more than 8 million people each year globally by the year 2030, with 80% of these deaths in the developing countries. This study aimed to determine the prevalence and associated factors of cigarette smoking among male university students in Muzaffarabad, Pakistan. A descriptive cross-sectional study was conducted among 542 male students at University of Azad Jammu & Kashmir in Muzaffarabad from July to December 2015. The socio-demographic characteristics and cigarette smoking behavior of the students were measured by using a standardized pre-tested self-administrated validated questionnaire in English. The overall prevalence of cigarette smoking among students was found to be 49.4%. The mean age of starting cigarette smoking was 19.2 2.73 years. Age, marital status and education were found significantly associted with cigarette smoking behavior (p-value<0.05). The most common reason for cigarette smoking was stress alleviation (35.0%) followed by peer pressure (24.5%). As cigarette smoking is considerably higher among students. There is a need to develop effective tobacco control measures among university students in Muzaffarabad.
Mubarak Hussain
Aija Zobena
Despite the detrimental impact of smoking to health, its prevalence remains high. Most students who smoke start to do so regularly around the age of 16-18. Although the proportion of smokers in Latvia is decreasing, the share of electronic cigarette users among young people is growing prematurely, which indicates a change of habits among young people. The aim of the study is to investigate the motives for starting smoking, the factors that contribute to smoking initiation and how high school students become “regular smokers” from “trying” tobacco products. In February 2019, two focus group discussions were organized to obtain information on young people's smoking experience. In each of them, high school students (aged over 18) and students took part. The participants of the focus group discussion were chosen by the “snowball” method. Social factors and the social and psychological characteristics of adolescents have a major impact on the transition from the first cigarette smoke...
Journal of Tropical Pediatrics
Shubhadeep Das
Turk J Med Sci
Sevgi ONCEL
Journal of King Abdulaziz University-Medical Sciences
Samar Alsaggaf
Loading Preview
Sorry, preview is currently unavailable. You can download the paper by clicking the button above.
RELATED PAPERS
Tobacco and Health
asiyeh yari
Humanities & Social Sciences Reviews
robab rahmati
Pakistan Journal of Medical and Health Sciences
saima afzal
Vicente MARTÍN SÁNCHEZ
Revista de Chimie
Corina Budin
prince Egyptian
Leyla Şenol
Meandros Medical and Dental Journal
Ecenur Topal
crazy man run
MOHD SADIQ SALMAN
Journal of Evolution of Medical and Dental Sciences
ishika chandra
Eurasian Journal of Pulmonology
Nurhan Sarioglu
Turkish Thoracic Journal/Türk Toraks Dergisi
Hilal Ozcebe
Tochukwu Igboanugo
RELATED TOPICS
- We're Hiring!
- Help Center
- Find new research papers in:
- Health Sciences
- Earth Sciences
- Cognitive Science
- Mathematics
- Computer Science
- Academia ©2024
235 Smoking Essay Topics & Examples
Looking for smoking essay topics? Being one of the most serious psychological and social issues, smoking is definitely worth writing about.
🏆 Best Smoking Essay Examples & Topic Ideas
🥇 good titles for smoking essay, 👍 best titles for research paper about smoking, ⭐ simple & easy health essay titles, 💡 interesting topics to write about health, ❓ essay questions about smoking.
In your essay about smoking, you might want to focus on its causes and effects or discuss why smoking is a dangerous habit. Other options are to talk about smoking prevention or to concentrate on the reasons why it is so difficult to stop smoking. Here we’ve gathered a range of catchy titles for research papers about smoking together with smoking essay examples. Get inspired with us!
Smoking is a well-known source of harm yet popular regardless, and so smoking essays should cover various aspects of the topic to identify the reasons behind the trend.
You will want to discuss the causes and effects of smoking and how they contributed to the persistent refusal of large parts of the population to abandon the habit, even if they are aware of the dangers of cigarettes. You should provide examples of how one may become addicted to tobacco and give the rationales for smokers.
You should also discuss the various consequences of cigarette use, such as lung cancer, and identify their relationship with the habit. By discussing both sides of the issue, you will be able to write an excellent essay.
Reasons why one may begin smoking, are among the most prominent smoking essay topics. It is not easy to begin to enjoy the habit, as the act of smoke inhalation can be difficult to control due to a lack of experience and unfamiliarity with the concept.
As such, people have to be convinced that the habit deserves consideration by various ideas or influences. The notion that “smoking is cool” among teenagers can contribute to the adoption of the trait, as can peer pressure.
If you can find polls and statistics on the primary factors that lead people to tweet, they will be helpful to your point. Factual data will identify the importance of each cause clearly, although you should be careful about bias.
The harmful effects of tobacco have been researched considerably more, with a large body of medical studies investigating the issue available to anyone.
Lung cancer is the foremost issue in the public mind because of the general worry associated with the condition and its often incurable nature, but smoking can lead to other severe illnesses.
Heart conditions remain a prominent consideration due to their lethal effects, and strokes or asthma deserve significant consideration, as well. Overall, smoking has few to no beneficial health effects but puts the user at risk of a variety of concerns.
As such, people should eventually quit once their health declines, but their refusal to do so deserves a separate investigation and can provide many interesting smoking essay titles.
One of the most prominent reasons why a person would continue smoking despite all the evidence of its dangers and the informational campaigns carried out to inform consumers is nicotine addiction.
The substance is capable of causing dependency, a trait that has led to numerous discussions of the lawfulness of the current state of cigarettes.
It is also among the most dangerous aspects of smoking, a fact you should mention.
Lastly, you can discuss the topics of alternatives to smoking in your smoking essay bodies, such as e-cigarettes, hookahs, and vapes, all of which still contain nicotine and can, therefore, lead to considerable harm. You may also want to discuss safe cigarette avoidance options and their issues.
Here are some additional tips for your essay:
- Dependency is not the sole factor in cigarette consumption, and many make the choice that you should respect consciously.
- Cite the latest medical research titles, as some past claims have been debunked and are no longer valid.
- Mortality is not the sole indicator of the issues associated with smoking, and you should take chronic conditions into consideration.
Find smoking essay samples and other useful paper samples on IvyPanda, where we have a collection of professionally written materials!
- How Smoking Is Harmful to Your Health The primary purpose of the present speech is to inform the audience about the detrimental effects of smoking. The first system of the human body that suffers from cigarettes is the cardiovascular system.
- Smoking: Problems and Solutions To solve the problem, I would impose laws that restrict adults from smoking in the presence of children. In recognition of the problems that tobacco causes in the country, The Canadian government has taken steps […]
- Conclusion of Smoking Should Be Banned on College Campuses Essay However, it is hard to impose such a ban in some colleges because of the mixed reactions that are held by different stakeholders about the issue of smoking, and the existing campus policies which give […]
- Should Smoking Be Banned in Public Places? Besides, smoking is an environmental hazard as much of the content in the cigarette contains chemicals and hydrocarbons that are considered to be dangerous to both life and environment.
- Smoking Cigarette Should Be Banned Ban on tobacco smoking has resulted to a decline in the number of smokers as the world is sensitized on the consequences incurred on 31st May.
- Causes and Effects of Smoking Some people continue smoking as a result of the psychological addiction that is associated with nicotine that is present in cigarettes.
- Should Cigarettes Be Banned? Essay Banning cigarette smoking would be of great benefit to the young people. Banning of cigarette smoking would therefore reduce stress levels in people.
- Advertisements on the Effect of Smoking Do not Smoke” the campaign was meant to discourage the act of smoking among the youngsters, and to encourage them to think beyond and see the repercussions of smoking.
- Smoking Cessation Programs Through the Wheel of Community Organizing The first step of the wheel is to listen to the community’s members and trying to understand their needs. After the organizer and the person receiving treatment make the connection, they need to understand how […]
- Smoking: Effects, Reasons and Solutions This presentation provides harmful health effects of smoking, reasons for smoking, and solutions to smoking. Combination therapy that engages the drug Zyban, the concurrent using of NRT and counseling of smokers under smoking cessation program […]
- On Why One Should Stop Smoking Thesis and preview: today I am privileged to have your audience and I intend to talk to you about the effects of smoking, and also I propose to give a talk on how to solve […]
- Tobacco Smoking and Its Dangers Sufficient evidence also indicates that smoking is correlated with alcohol use and that it is capable of affecting one’s mental state to the point of heightening the risks of development of disorders.
- Smoking and Its Negative Effects on Human Beings Therefore, people need to be made aware of dental and other health problems they are likely to experience as a result of smoking.
- Smoking and Its Effects on Human Body The investigators explain the effects of smoking on the breath as follows: the rapid pulse rate of smokers decreases the stroke volume during rest since the venous return is not affected and the ventricles lose […]
- Smoking Among Teenagers as Highlighted in Articles The use of tobacco through smoking is a trend among adolescents and teenagers with the number of young people who involve themselves in smoking is growing each day.
- Quitting Smoking: Strategies and Consequences Thus, for the world to realize a common positive improvement in population health, people must know the consequences of smoking not only for the smoker but also the society. The first step towards quitting smoking […]
- “Thank You For Smoking” by Jason Reitman Film Analysis Despite the fact that by the end of the film the character changes his job, his nature remains the same: he believes himself to be born to talk and convince people.
- Hookah Smoking and Its Risks The third component of a hookah is the hose. This is located at the bottom of the hookah and acts as a base.
- Teenage Smoking and Solution to This Problem Overall, the attempts made by anti-smoking campaigners hardly yield any results, because they mostly focus on harmfulness of tobacco smoking and the publics’ awareness of the problem, itself, but they do not eradicate the underlying […]
- Social Marketing: The Truth Anti-Smoking Campaign The agreement of November 1998 between 46 states, five territories of the United States, the District of Columbia, and representatives of the tobacco industry gave start to the introduction of the Truth campaign.
- Cigarette Smoking in Public Places Those who argue against the idea of banning the smoking are of the opinion that some of them opt to smoke due to the stress that they acquire at their work places.
- Ban of Tobacco Smoking in Jamaica The first part of the paper will address effects of tobacco smoking on personal health and the economy. Cognizant of its international obligation and the aforementioned health effects of tobacco smoke, Jamaica enacted a law […]
- Should Smoking Tobacco Be Classified As an Illegal Drug? Although this is the case, the tobacco industry is one of the most profitable industries, a fact that has made it very hard for the government to illegalize the use of tobacco products.
- A Peer Intervention Program to Reduce Smoking Rates Among LGBTQ Therefore, the presumed results of the project are its introduction into the health care system, which will promote a healthy lifestyle and diminish the level of smoking among LGBTQ people in the SESLHD.
- Health Promotion for Smokers The purpose of this paper is to show the negative health complications that stem from tobacco use, more specifically coronary heart disease, and how the health belief model can help healthcare professionals emphasize the importance […]
- Gender-Based Assessment of Cigarette Smoking Harm Thus, the following hypothesis is tested: Women are more likely than men to believe that smoking is more harmful to health.
- Hazards of Smoking and Benefits of Cessation Prabhat Jha is the author of the article “The Hazards of Smoking and the Benefits of Cessation,” published in a not-for-profit scientific journal, eLife, in 2020.
- The Impact of Warning Labels on Cigarette Smoking The regulations requiring tobacco companies to include warning labels are founded on the need to reduce nicotine intake, limit cigarette dependence, and mitigate the adverse effects associated with addiction to smoking.
- Psilocybin as a Smoking Addiction Remedy Additionally, the biotech company hopes to seek approval from FDA for psilocybin-based therapy treatment as a cigarette smoking addiction long-term remedy.
- Investing Savings from Quitting Smoking: A Financial Analysis The progression of interest is approximately $50 per year, and if we assume n equal to 45 using the formula of the first n-terms of the arithmetic progression, then it comes out to about 105 […]
- Smoking as a Community Issue: The Influence of Smoking A review of the literature shows the use of tobacco declined between 1980 and 2012, but the number of people using tobacco in the world is increasing because of the rise in the global population.
- Smoking Public Education Campaign Assessment The major influence of the real cost campaign was to prevent the initiation of smoking among the youth and prevent the prevalence of lifelong smokers.
- Quitting Smoking and Related Health Benefits The regeneration of the lungs will begin: the process will touch the cells called acini, from which the mucous membrane is built. Therefore, quitting the habit of smoking a person can radically change his life […]
- Smoking and Stress Among Veterans The topic is significant to explore because of the misconception that smoking can alleviate the emotional burden of stress and anxiety when in reality, it has an exacerbating effect on emotional stress.
- Smoking as a Predictor of Underachievement By comparing two groups smoking and non-smoking adolescents through a parametric t-test, it is possible to examine this assumption and draw conclusions based on the resulting p-value.
- Smoking and the Pandemic in West Virginia In this case, the use of the income variable is an additional facet of the hypothesis described, allowing us to evaluate whether there is any divergence in trends between the rich and the poor.
- Anti-Smoking Policy in Australia and the US The anti-smoking policy is to discourage people from smoking through various means and promotion of a healthy lifestyle, as well as to prevent the spread of the desire to smoke.
- Smoking Prevalence in Bankstown, Australia The secondary objective of the project was to gather and analyze a sufficient amount of auxiliary scholarly sources on smoking cessation initiatives and smoking prevalence in Australia.
- Drug Addiction in Teenagers: Smoking and Other Lifestyles In the first part of this assignment, the health problem of drug addiction was considered among teens and the most vulnerable group was established.
- Aspects of Anti-Smoking Advertising Thus, it is safe to say that the authors’ main and intended audience is the creators of anti-smoking public health advertisements.
- Anti-Smoking Communication Campaign’s Analysis Defining the target audience for an anti-smoking campaign is complicated by the different layers of adherence to the issue of the general audience of young adults.
- Smoking Cessation Project Implementation In addition, the review will include the strengths and weaknesses of the evidence presented in the literature while identifying gaps and limitations.
- Smoking Cessation and Health Promotion Plan Patients addicted to tobacco are one of the major concerns of up-to-date medicine as constant nicotine intake leads to various disorders and worsens the health state and life quality of the users.
- Maternal and Infant Health: Smoking Prevention Strategies It is known that many women know the dangers of smoking when pregnant and they always try to quit smoking to protect the lives of themselves and the child.
- Peer Pressure and Smoking Influence on Teenagers The study results indicate that teenagers understand the health and social implications of smoking, but peer pressure contributes to the activity’s uptake.
- Smoking: Benefits or Harms? Hundreds of smokers every day are looking for a way to get rid of the noose, which is a yoke around the neck, a cigarette.
- The Culture of Smoking Changed in Poland In the 1980-90s, Poland faced the challenge of being a country with the highest rates of smoking, associated lung cancer, and premature mortality in the world.
- The Stop Smoking Movement Analysis The paper discusses the ideology, objective, characteristics, context, special techniques, organization culture, target audience, media strategies, audience reaction, counter-propaganda and the effectiveness of the “Stop Smoking” Movement.”The Stop Smoking” campaign is a prevalent example of […]
- Health Promotion Plan: Smokers in Mississippi The main strategies of the training session are to reduce the number of smokers in Mississippi, conduct a training program on the dangers of smoking and work with tobacco producers.
- Smoking Health Problem Assessment The effects of smoking correlate starkly with the symptoms and diseases in the nursing practice, working as evidence of the smoking’s impact on human health.
- Integration of Smoking Cessation Into Daily Nursing Practice Generally, smoking cessation refers to a process structured to help a person to discontinue inhaling smoked substances. It can also be referred to as quitting smoking.
- E-Cigarettes and Smoking Cessation Many people argue that e-cigarettes do not produce secondhand smoke. They believe that the e-fluids contained in such cigarettes produce vapor and not smoke.
- Introducing Smoking Cessation Program: 5 A’s Intervention Plan The second problem arises in an attempt to solve the issue of the lack of counseling in the unit by referring patients to the outpatient counseling center post-hospital discharge to continue the cessation program.
- Outdoor Smoking Ban in Public Areas of the Community These statistics have contributed to the widespread efforts to educate the public regarding the need to quit smoking. However, most of the chronic smokers ignore the ramifications of the habit despite the deterioration of their […]
- Nicotine Replacement Therapy for Adult Smokers With a Psychiatric Disorder The qualitative research methodology underlines the issue of the lack of relevant findings in the field of nicotine replacement therapy in people and the necessity of treatment, especially in the early stages of implementation.
- Smoking and Drinking: Age Factor in the US As smoking and drinking behavior were both strongly related to age, it could be the case that the observed relationship is due to the fact that older pupils were more likely to smoke and drink […]
- Smoking Cessation Clinic Analysis The main aim of this project is to establish a smoking cessation clinic that will guide smoker through the process of quitting smoking.
- Cigarette Smoking Among Teenagers in the Baltimore Community, Maryland The paper uses the Baltimore community in Maryland as the area to focus the event of creating awareness of cigarette smoking among the teens of this community.
- Advocating for Smoking Cessation: Health Professional Role Health professionals can contribute significantly to tobacco control in Australia and the health of the community by providing opportunities for smoking patients to quit smoking.
- Lifestyle Management While Quitting Smoking Realistically, not all of the set goals can be achieved; this is due to laxity in implementing them and the associated difficulty in letting go of the past lifestyle.
- Smoking in the Actuality The current use of aggressive marketing and advertising strategies has continued to support the smoking of e-cigarettes. The study has also indicated that “the use of such e-cigarettes may contribute to the normalization of smoking”.
- Analysis of the Family Smoking Prevention and Tobacco Control Act The law ensures that the FDA has the power to tackle issues of interest to the public such as the use of tobacco by minors.
- “50-Year Trends in Smoking-Related Mortality in the United States” by Thun et al. Thun is affiliated with the American Cancer Society, but his research interests cover several areas. Carter is affiliated with the American Cancer Society, Epidemiology Research Program.
- Pulmonology: Emphysema Caused by Smoking The further development of emphysema in CH can lead to such complications caused by described pathological processes as pneumothorax that is associated with the air surrounding the lungs.
- Smoking and Lung Cancer Among African Americans Primarily, the research paper provides insight on the significance of the issue to the African Americans and the community health nurses.
- Health Promotion and Smoking Cessation I will also complete a wide range of activities in an attempt to support the agency’s goals. As well, new studies will be conducted in order to support the proposed programs.
- Maternal Mental Health and Prenatal Smoking It was important to determine the variables that may lead to postpartum relapse or a relapse during the period of pregnancy. It is important to note that the findings are also consistent with the popular […]
- Nursing Interventions for Smoking Cessation For instance, the authors are able to recognize the need to classify the level of intensity in respect to the intervention that is employed by nurses towards smoking cessation.
- Smoking and Cancer in the United States In this research study, data on tobacco smoking and cancer prevalence in the United States was used to determine whether cancer in the United States is related to tobacco smoking tobacco.
- Marketing Plan: Creating a Smoking Cessation Program for Newton Healthcare Center The fourth objective is to integrate a smoking cessation program that covers the diagnosis of smoking, counseling of smokers, and patient care system to help the smokers quit their smoking habits. The comprehensive healthcare needs […]
- Risks of Smoking Cigarettes Among Preteens Despite the good news that the number of preteen smokers has been significantly reducing since the 1990s, there is still much to be done as the effects of smoking are increasingly building an unhealthy population […]
- Public Health Education: Anti-smoking Project The workshop initiative aimed to achieve the following objectives: To assess the issues related to smoking and tobacco use. To enhance the health advantages of clean air spaces.
- Healthy People Program: Smoking Issue in Wisconsin That is why to respond to the program’s effective realization, it is important to discuss the particular features of the target population in the definite community of Wisconsin; to focus on the community-based response to […]
- Health Campaign: Smoking in the USA and How to Reduce It That is why, the government is oriented to complete such objectives associated with the tobacco use within the nation as the reduction of tobacco use by adults and adolescents, reduction of initiation of tobacco use […]
- Smoking Differentials Across Social Classes The author inferred her affirmations from the participant’s words and therefore came to the right conclusion; that low income workers had the least justification for smoking and therefore took on a passive approach to their […]
- Cigarette Smoking Side Effects Nicotine is a highly venomous and addictive substance absorbed through the mucous membrane in the mouth as well as alveoli in the lungs.
- Long-Term Effects of Smoking The difference between passive smoking and active smoking lies in the fact that, the former involves the exposure of people to environmental tobacco smoke while the latter involves people who smoke directly.
- Smoking Cessation Program Evaluation in Dubai The most important program of this campaign is the Quit and Win campaign, which is a unique idea, launched by the DHCC and is in the form of an open contest.
- Preterm Birth and Maternal Smoking in Pregnancy The major finding of the discussed research is that both preterm birth and maternal smoking during pregnancy contribute, although independently, to the aortic narrowing of adolescents.
- Enforcement of Michigan’s Non-Smoking Law This paper is aimed at identifying a plan and strategy for the enforcement of the Michigan non-smoking law that has recently been signed by the governor of this state.
- Smoking Cessation for Patients With Cardio Disorders It highlights the key role of nurses in the success of such programs and the importance of their awareness and initiative in determining prognosis.
- Legalizing Electronic Vaping as the Means of Curbing the Rates of Smoking However, due to significantly less harmful effects that vaping produces on health and physical development, I can be considered a legitimate solution to reducing the levels of smoking, which is why it needs to be […]
- Inequality and Discrimination: Impact on LGBTQ+ High School Students Consequently, the inequality and discrimination against LGBTQ + students in high school harm their mental, emotional, and physical health due to the high level of stress and abuse of various substances that it causes.
- Self-Efficacy and Smoking Urges in Homeless Individuals Pinsker et al.point out that the levels of self-efficacy and the severity of smoking urges change significantly during the smoking cessation treatment.
- “Cigarette Smoking: An Overview” by Ellen Bailey and Nancy Sprague The authors of the article mentioned above have presented a fair argument about the effects of cigarette smoking and debate on banning the production and use of tobacco in America.
- “The Smoking Plant” Project: Artist Statement It is the case when the art is used to pass the important message to the observer. The live cigarette may symbolize the smokers while the plant is used to denote those who do not […]
- Dangers of Smoking While Pregnant In this respect, T-test results show that mean birthweight of baby of the non-smoking mother is 3647 grams, while the birthweight of smoking mother is 3373 grams. Results show that gestation value and smoking habit […]
- The Cultural Differences of the Tobacco Smoking The Middle East culture is connected to the hookah, the Native American cultures use pipes, and the Canadian culture is linked to cigarettes.
- Ban on Smoking in Enclosed Public Places in Scotland The theory of externality explains the benefit or cost incurred by a third party who was not a party to the reasoning behind the benefit or cost. This will also lead to offer of a […]
- How Smoking Cigarettes Effects Your Health Cigarette smoking largely aggravates the condition of the heart and the lung. In addition, the presence of nicotine makes the blood to be sticky and thick leading to damage to the lining of the blood […]
- Alcohol and Smoking Abuse: Negative Physical and Mental Effects The following is a range of effects of heavy alcohol intake as shown by Lacoste, they include: Neuropsychiatric or neurological impairment, cardiovascular, disease, liver disease, and neoplasm that is malevolent.
- Smoking Prohibition: Local Issues, Personal Views This is due to the weakening of blood vessels in the penis. For example, death rate due to smoking is higher in Kentucky than in other parts of the country.
- Tobacco Smoking: Bootleggers and Baptists Legislation or Regulation The issue is based on the fact that tobacco smoking also reduces the quality of life and ruins the body in numerous ways.
- Ban Smoking in Cars Out of this need, several regulations have been put in place to ensure children’s safety in vehicles is guaranteed; thus, protection from second-hand smoke is an obvious measure that is directed towards the overall safety […]
- Smoking: Causes and Effects Considering the peculiarities of a habit and of a disease, smoking can be considered as a habit rather than a disease.
- Smoking and Its Effect on the Brain Since the output of the brain is behavior and thoughts, dysfunction of the brain may result in highly complex behavioral symptoms. The work of neurons is to transmit information and coordinate messengers in the brain […]
- Smoking Causes and Plausible Arguments In writing on the cause and effect of smoking we will examine the issue from the point of view of temporal precedence, covariation of the cause and effect and the explanations in regard to no […]
- Summary of “Smokers Get a Raw Deal” by Stanley Scott Lafayette explains that people who make laws and influence other people to exercise these laws are obviously at the top of the ladder and should be able to understand the difference between the harm sugar […]
- Smoking Qualitative Research: Critical Analysis Qualitative research allows researchers to explore a wide array of dimensions of the social world, including the texture and weave of everyday life, the understandings, experiences and imaginings of our research participants, the way that […]
- Motivational Interviewing as a Smoking Cessation Intervention for Patients With Cancer The dependent variable is the cessation of smoking in 3 months of the interventions. The study is based on the author’s belief that cessation of smoking influences cancer-treated patients by improving the efficacy of treatment.
- Factors Affecting the Success in Quitting Smoking of Smokers in West Perth, WA Australia Causing a wide array of diseases, health smoking is the second cause of death in the world. In Australia, the problem of smoking is extremely burning due to the high rates of diseases and deaths […]
- Media Effects on Teen Smoking But that is not how an adult human brain works, let alone the young and impressionable minds of teenagers, usually the ads targeted at the youth always play upon elements that are familiar and appealing […]
- Partnership in Working About Smoking and Tobacco Use The study related to smoking and tobacco use, which is one of the problematic areas in terms of the health of the population.
- Causes and Effects of Smoking in Public The research has further indicated that the carcinogens are in higher concentrations in the second hand smoke rather than in the mainstream smoke which makes it more harmful for people to smoke publicly.
- Quitting Smoking: Motivation and Brain As these are some of the observed motivations for smoking, quitting smoking is actually very easy in the sense that you just have to set your mind on quitting smoking.
- Health Effects of Tobacco Smoking in Hispanic Men The Health Effects of Tobacco Smoking can be attributed to active tobacco smoking rather than inhalation of tobacco smoke from environment and passive smoking.
- Smoking in Adolescents: A New Threat to the Society Of the newer concerns about the risks of smoking and the increase in its prevalence, the most disturbing is the increase in the incidences of smoking among the adolescents around the world.
- Smoking and Youth Culture in Germany The report also assailed the Federal Government for siding the interest of the cigarette industry instead of the health of the citizens.
- New Jersey Legislation on Smoking The advantages and disadvantages of the legislation were discussed in this case because of the complexity of the topic at hand as well as the potential effects of the solution on the sphere of public […]
- Environmental Health: Tabaco Smoking and an Increased Concentration of Carbon Monoxide The small size of the town, which is around 225000 people, is one of the reasons for high statistics in diseases of heart rate.
- Advanced Pharmacology: Birth Control for Smokers The rationale for IUD is the possibility to control birth without the partner’s participation and the necessity to visit a doctor just once for the device to be implanted.
- Legislation Reform of Public Smoking Therefore, the benefit of the bill is that the health hazard will be decreased using banning smoking in public parks and beaches.
- Smoking Bans: Protecting the Public and the Children of Smokers The purpose of the article is to show why smoking bans aim at protecting the public and the children of smokers.
- Clinical Effects of Cigarette Smoking Smoking is a practice that should be avoided or controlled rigorously since it is a risk factor for diseases such as cancer, affects the health outcomes of direct and passive cigarette users, children, and pregnant […]
- Public Health and Smoking Prevention Smoking among adults over 18 years old is a public health issue that requires intervention due to statistical evidence of its effects over the past decades.
- Smoking Should Be Banned Internationally The questions refer to the knowledge concerning the consequences of smoking and the opinions on smoking bans. 80 % of respondents agree that smoking is among the leading causes of death and 63, 3 % […]
- Microeconomics: Cigarette Taxes and Public Smoking Ban The problem of passive smoking will be minimized when the number of smokers decreases. It is agreeable that the meager incomes of such families will be used to purchase cigarettes.
- Tobacco Debates in “Thank You for Smoking” The advantage of Nick’s strategy is that it offers the consumer a role model to follow: if smoking is considered to be ‘cool’, more people, especially young ones, will try to become ‘cool’ using cigarettes.
- Alcohol and Smoking Impact on Cancer Risk The research question is to determine the quantity of the impact that different levels of alcohol ingestion combined with smoking behavioral patterns make on men and women in terms of the risks of cancer.
- Indoor Smoking Restriction Effects at the Workplace Regrettably, they have neglected research on the effect of the legislation on the employees and employers. In this research, the target population will be the employees and employers of various companies.
- Hypnotherapy Session for Smoking Cessation When I reached the age of sixty, I realized that I no longer wanted to be a smoker who was unable to take control of one’s lifestyle.
- Vancouver Coastal Health Smoking Cessation Program The present paper provides an evaluation of the Vancouver Coastal Health smoking cessation program from the viewpoint of the social cognitive theory and the theory of planned behavior.
- Smoking Experience and Hidden Dangers When my best college friend Jane started smoking, my eyes opened on the complex nature of the problem and on the multiple negative effects of smoking both on the smoker and on the surrounding society.
- South Illinois University’s Smoking Ban Benefits The purpose of this letter is to assess the possible benefits of the plan and provide an analysis of the costs and consequences of the smoking ban introduction.
- Smoking Cessation in Patients With COPD The strategy of assessing these papers to determine their usefulness in EBP should include these characteristics, the overall quality of the findings, and their applicability in a particular situation. The following article is a study […]
- Smoking Bans: Preventive Measures There have been several public smoking bans that have proved to be promising since the issue of smoking prohibits smoking in all public places. This means it is a way of reducing the exposure to […]
- Ban Smoking Near the Child: Issues of Morality The decision to ban smoking near the child on father’s request is one of the demonstrative examples. The father’s appeal to the Supreme Court of California with the requirement to prohibit his ex-wife from smoking […]
- The Smoking Ban: Arguments Comparison The first argument against banning smoking employs the idea that smoking in specially designated areas cannot do harm to the health of non-smokers as the latter are supposed to avoid these areas.
- Smoking Cessation and Patient Education in Nursing Pack-years are the concept that is used to determine the health risks of a smoking patient. The most important step in the management plan is to determine a date when the man should quit smoking.
- Philip Morris Company’s Smoking Prevention Activity Philip Morris admits the existence of scientific proof that smoking leads to lung cancer in addition to other severe illnesses even after years of disputing such findings from health professionals.
- Virginia Slims’ Impact on Female Smokers’ Number Considering this, through the investigation of Philip Morris’ mission which it pursued during the launch of the Virginia Slims campaign in 1968-1970 and the main regulatory actions undertaken by the Congress during this period, the […]
- Cigarette Smoking and Parkinson’s Disease Risk Therefore, given the knowledge that cigarette smoking protects against the disease, it is necessary to determine the validity of these observations by finding the precise relationship between nicotine and PD.
- Tuberculosis Statistics Among Cigarette Smokers The proposal outlines the statistical applications of one-way ANOVA, the study participants, the variables, study methods, expected results and biases, and the practical significance of the expected results.
- Smoking Habit, Its Causes and Effects Smoking is one of the factors that are considered the leading causes of several health problems in the current society. Smoking is a habit that may be easy to start, but getting out of this […]
- Smoking Ban and UK’s Beer Industry However, there is an intricate type of relationship between the UK beer sector, the smoking ban, and the authorities that one can only understand by going through the study in detail The history of smoking […]
- Status of Smoking around the World Economic factors and level of education have contributed a lot to the shift of balance in the status of smoking in the world.
- Redwood Associates Company’s Smoking Ethical Issues Although employees are expected to know what morally they are supposed to undertake at their work place, it is the responsibility of the management and generally the Redwood’s hiring authority to give direction to its […]
- Smokers’ Campaign: Finding a Home for Ciggy Butts When carrying out the campaign, it is important to know what the situation on the ground is to be able to address the root cause of the problem facing the population.
- Mobile Applications to Quit Smoking A critical insight that can be gleaned from the said report is that one of the major factors linked to failure is the fact that smokers were unable to quit the habit on their own […]
- Behavior Modification Technique: Smoking Cessation Some of its advantages include: its mode of application is in a way similar to the act of smoking and it has very few side effects.
- Effects of Thought Suppression on Smoking Behavior In the article under analysis called I suppress, Therefore I smoke: Effects of Thought Suppression on Smoking Behavior, the authors dedicate their study to the evaluation of human behavior as well as the influence of […]
- Suppressing Smoking Behavior and Its Effects The researchers observed that during the first and the second weeks of the suppressed behavior, the participants successfully managed to reduce their intake of cigarettes.
- Smoking Cessation Methods These methods are a part of NRT or nicotine replacement therapy, they work according to the principle of providing the smoker with small portions of nicotine to minimize the addiction gradually and at the same […]
- Understanding Advertising: Second-Hand Smoking The image of the boy caught by the smoke is in the center of the picture, and it is in contrast with the deep black background.
- People Should Quit Smoking Other counseling strategies such as telephone calls and social support also serves the ultimate goal of providing a modern approach in which counseling can be tailored to suit the counseling needs of an individual smoker. […]
- Importance of Quitting Smoking As such, quitting smoking is important since it helps relief the worry and the fear associated with possibility of developing cancer among other smoking-related illnesses. It is therefore important to quit smoking if the problems […]
- Anti-Smoking Campaign in Canada This is not the first attempt that the federal government of Canada intends to make in reducing the prevalence of smoking in the country.
- Electronic Cigarettes: Could They Help University Students Give Smoking Up? Electronic Cigarettes An electronic cigarette is an electronic device that simulates the act of smoking by producing a mist which gives the physical sensation and often the flavor and the nicotine just as the analog […]
- The Change of my Smoking Behavior With the above understanding of my social class and peer friends, I was able to create a plan to avoid them in the instances that they were smoking.
- Psychosocial Smoking Rehabilitation According to Getsios and Marton most of the economic models that evaluate the effects of smoke quitting rehabilitation consider the influence of a single quit attempt.
- The Program on Smoking Cessation for Employees Due to the fact that the main purpose of the program on smoking cessation consisted in improving healthy lifestyles of their employees, the focus on cost reduction and insurance seems to be irrelevant.
- Tips From Former Smokers (Campaign) Over the years, the campaigns have led to both the increase and the decrease of smoking all over the world. The second type of anti-smoking campaign employed was the use of celebrities to encourage people […]
- Combating Smoking: Taxation Policies vs. Education Policies This is a considerable provision in the realms of health; hence, the efforts created by the government to curb this trend should be supported fully. In this regard, there is need to reduce the mentioned […]
- The Program to Quit Smoking The second stage of the evaluation proves revealed the benefits of the program for the hospital in terms of discount rates for employees, age categories involved in the program. This process consists in selection of […]
- Smoking Culture in Society Smoking culture refers to the practice of smoking tobacco by people in the society for the sheer satisfaction and delight it offers.
- Possible Smoking Policies in Florida Majority also think that went it comes to workplaces hotels and bars it would be more appropriate to provide specific smoking zones as opposed to total bans The implications of the policy adopted therefore affect […]
- Smoking Ban in the State of Florida These are the Total Ban Policy, the Partial Ban policy and the Liberated Smoking policy. The policy is authoritarian and ignores the interests of the smokers.
- Core Functions of Public Health in the Context of Smoking and Heart Disease In the relation to our problem, heart attacks and smoking, it is important to gather the information devoted to the number of people who suffered from heart attacks and indicate the percentage rate of those […]
- Smoking: Pathophysiological Effects In addition to the effects of smoking on the various body organs including the heart and lungs, smoking has also been shown to have adverse effects on the brain resulting to a compromise of the […]
- Putting Out the Fires: Will Higher Taxes Reduce the Onset of Youth Smoking? According to the article under consideration, increase in price of cigarettes can positively or negatively affect the rate of smoking among the youth.
- Smoking Bans in US
- Smoking as Activity Enhancer: Schizophrenia and Gender
- Health Care Costs for Smokers
- Medical Coverage for Smoking Related Diseases
- Exposure to mass media proliferate smoking
- The Realm of reality: Smoking
- Ethical Problem of Smoking
- The Rate of Smoking Among HIV Positive Cases.
- Studying the Government’s Anti-Smoking Measures
- Smoking Should Be Banned In the United States
- Effectiveness of Cognitive Behavioral Theory on Smoking Cessation
- Effectiveness of the Cognitive Behavioral Therapy for Smoking Cessation
- Wayco Company’s Non-smoking Policy
- Adverse Aspects of Smoking
- Negative Impacts of Smoking on Individuals and Society
- Dealing With the Increase in the Number of Smokers Between Ages 17 and 45
- Cannabis Smoking in Canada
- Smoking Ban in the United States of America
- Dangers of Smoking Campaign
- Smoking Ban in New York
- Smoking and Adolescents
- Trends in Smoking Prevalence by Race/Ethnicity
- Business Ethics: Smoking Issue
- Where Does the Path to Smoking Addiction Start?
- Public Health Communication: Quit Smoking
- Are Estimated Peer Effects on Smoking Robust?
- Are There Safe Smoking and Tobacco Options?
- What Are the Health Risks of Smoking?
- Does Cigarette Smoking Affect Body Weight?
- Does Cigarette Smuggling Prop Up Smoking Rates?
- What Foods Help You Quit Smoking?
- How Can People Relax Without Smoking?
- Does Education Affect Smoking Behaviors?
- Is Vaping Worse Than Smoking?
- Do Movies Affect Teen Smoking?
- What Is Worse: Drinking or Smoking?
- Does Smoking Affect Breathing Capacity?
- Does Smoking Cause Lung Cancer?
- Does Having More Children Increase the Likelihood of Parental Smoking?
- Does Smoking Cigarettes Relieve Stress?
- Does Time Preference Affect Smoking Behavior?
- How Does Smoking Affect Cardiovascular Endurance?
- How Hypnosis Can Help You Quit Smoking?
- How Does Smoking Affect Brain?
- How Nicotine Affects Your Quit Smoking Victory?
- How Does Secondhand Smoking Affect Us?
- Why Is Smoking Addictive?
- How Smoking Bans Are Bad for Business?
- Why Smoking Should Not Be Permitted in Restaurants?
- Why Public Smoking Should Be Banned?
- Why Has Cigarette Smoking Become So Prominent Within the American Culture?
- What Makes Smoking and Computers Similar?
- Does Smoking Affect Schooling?
- What Effects Can Cigarette Smoking Have on the Respiratory System?
- What Are the Most Prevalent Dangers of Smoking and Drinking?
- Social Security Paper Topics
- Drugs Titles
- Cannabis Essay Titles
- Global Issues Essay Topics
- Cardiovascular Diseases Titles
- Marijuana Ideas
- NHS Research Ideas
- Hypertension Topics
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2024, February 29). 235 Smoking Essay Topics & Examples. https://ivypanda.com/essays/topic/smoking-essay-examples/
"235 Smoking Essay Topics & Examples." IvyPanda , 29 Feb. 2024, ivypanda.com/essays/topic/smoking-essay-examples/.
IvyPanda . (2024) '235 Smoking Essay Topics & Examples'. 29 February.
IvyPanda . 2024. "235 Smoking Essay Topics & Examples." February 29, 2024. https://ivypanda.com/essays/topic/smoking-essay-examples/.
1. IvyPanda . "235 Smoking Essay Topics & Examples." February 29, 2024. https://ivypanda.com/essays/topic/smoking-essay-examples/.
Bibliography
IvyPanda . "235 Smoking Essay Topics & Examples." February 29, 2024. https://ivypanda.com/essays/topic/smoking-essay-examples/.
- Help & Support
- Quit Smoking
- Tobacco Facts
Tobacco Use Among Children and Teens
Cigarette smoking during childhood and adolescence causes significant health problems among young people, including an increase in the number and severity of respiratory illnesses, decreased physical fitness and potential effects on lung growth and function. 1
Most importantly, this is when an addiction to smoking takes hold, often lasting into and sometimes throughout adulthood. Among adults who have ever smoked daily, 87% had tried their first cigarette by the time they were 18 years of age, and 95% had by age 21. 2
Key Facts about Tobacco Use among Children and Teenagers
- Every day, almost 2,500 children under 18 years of age try their first cigarette, and more than 400 of them will become new, regular daily smokers. 3 Half of them will ultimately die from their habit. 4
- People who start smoking at an early age are more likely to develop a severe addiction to nicotine than those who start at a later age. Of adolescents who have smoked at least 100 cigarettes in their lifetime, most of them report that they would like to quit, but are not able to do so. 5
- If current tobacco use patterns persist, an estimated 5.6 million of today’s youth under age 18 eventually will die prematurely from a smoking-related disease. 6
Prevalence of Tobacco Use among Children and Teenagers
- In 2015, 9.3% of high school students reported smoking cigarettes in the last 30 days, down 74% from 36.4% in 1997 when rates peaked after increasing throughout the first half of the 1990s. 7
- In 2015, 2.3% of middle school students smoked cigarettes in the last 30 days. 7
- Rates of overall tobacco use remain high, however. In 2015, 25.3% of high school students and 7.4% of middle school students used a tobacco product. 7
- Among high school students in 2015, the most prevalent forms of tobacco used were electronic cigarettes (16%), cigarettes (9.3%), cigars (8.6%) and hookah (7.2%). 7
- In 2015, about half of middle and high school students reported using two or more tobacco products in the past 30 days. 7
- Since 1990, teenagers and young adults have had the highest rates of maternal smoking during pregnancy. In 2014, 10.2% of female teens aged 15 to 19 and 13% of women aged 20 to 24 smoked during pregnancy. 8
- In 2014, around 62% of current smokers in both middle and high school seriously thought about quitting. Seventy percent of middle school and 59% of high school current smokers had tried to quit smoking for one day or more. 9
Additional Facts about Tobacco Use among Children and Teenagers
- Menthol cigarette use is more common among younger and newer teen smokers. 10 This is due to young smokers perceiving menthol cigarettes as less harsh and easier to smoke. 11
- One study found that teens exposed to the greatest amount of smoking in movies were 2.6 times more likely to start smoking themselves compared with teens who watched the least amount of smoking in movies. 12
- The good news is that help is available for teen smokers who want to quit. The American Lung Association’s Not-On-Tobacco (N-O-T) program is designed for 14- to 19-year-old smokers who want to quit. Contact your local American Lung Association office to find out if N-O-T is available in your area.
Learn about the American Lung Association’s programs to help you or a loved one quit smoking , and join our advocacy efforts to reduce tobacco use and exposure to secondhand smoke. Visit Lung.org or call the Lung HelpLine at 1-800-LUNGUSA (1-800-586-4872).
U.S. Department of Health and Human Services. Preventing Tobacco Use Among Young People: A Report of the Surgeon General, 1994
Substance Abuse and Mental Health Services Administration. National Survey on Drug Use and Health, 2014. Analysis by the American Lung Association Epidemiology and Statistics Unit Using SPSS Software.
Substance Abuse and Mental Health Services Administration. 2015 National Survey on Drug Use and Health: Detailed Tables. 2016.
Centers for Disease Control and Prevention. Office on Smoking and Health. Sustaining State Programs for Tobacco Control: State Data Highlights, 2006. Accessed on June 9, 2008.
American Legacy Foundation. 2000. National Youth Tobacco Survey. 2001.
U.S. Department of Health and Human Services. The Health Consequences of Smoking—50 Years of Progress: A Report of the Surgeon General, 2014.
Centers for Disease Control and Prevention. Tobacco Use Among Middle and High School Students — United States, 2011–2015. Morbidity and Mortality Weekly Report. April 15, 2016; 65(14):361-7.
Centers for Disease Control and Prevention. National Center for Health Statistics. CDC WONDER On-line Database, Natality public-use data 2007-2014, 2016.
Centers for Disease Control and Prevention. National Youth Tobacco Survey, 2014. Analysis by the American Lung Association Epidemiology and Statistics Unit using SPSS software.
Hersey JC, Nonnemaker JM, Homsi G. Menthol Cigarettes Contribute to the Appeal and Addiction Potential of Smoking for Youth. Nicotine & Tobacco Research. 2010; 12(Suppl 2):S136–S146.
Klausner K. Menthol Cigarettes and Smoking Initiation: A Tobacco Industry Perspective. Tobacco Control. 2011; 20(Supp 2):ii12–ii19.
Lee YO, Glantz SA. Putting the Pieces Together. Tobacco Control. 2011; 20(Suppl 2):ii1–ii7.
Sargent JD et al. Exposure to Movie Smoking: Its Relations to Smoking Initiation Among US Adolescents. Pediatrics. November 5, 2005; 116(5):1183-91.
Page last updated: June 7, 2024
A Breath of Fresh Air In Your Inbox
Join over 700,000 people who receive the latest news about lung health, including research, lung disease, air quality, quitting tobacco, inspiring stories and more!
Thanks for submitting your email.
Make a Donation
Your tax-deductible donation funds lung disease and lung cancer research, new treatments, lung health education, and more.
Become a Lung Health Insider
Thank you! You will now receive email updates from the American Lung Association.
Select Your Location
Select your location to view local American Lung Association events and news near you.
Change Language
Lung helpline.
Talk to our lung health experts at the American Lung Association. Our service is free and we are here to help you.
1-800-LUNG-USA
(1-800-586-4872)

- All topics A-Z
- Grammar
- Vocabulary
- Speaking
- Reading
- Listening
- Writing
- Pronunciation
- Virtual Classroom
- Worksheets by season
- 600 Creative Writing Prompts
- Warmers, fillers & ice-breakers
- Coloring pages to print
- Flashcards
- Classroom management worksheets
- Emergency worksheets
- Revision worksheets
- Resources we recommend
Smoking Essay Examples & Topics
The Harmful Effects of Smoking on Human Health and Society1. Introduction Tobacco use represents a significant burden of death, disease, and economic cost around the world—particularly in low- and middle-income countries. Smoking-related diseases such as lung cancer, heart disease, and chronic obstructive pulmonary diseases are among the most common and deadly health risks. Smoking is spreading throughout many countries in the world due to the increasing number of young people. Mass media likes to focus on spreading the realization of the negative eff ... The Impact of Tobacco Use on Public Health and Society1. Introduction to Tobacco Use and Its Prevalence The use of any form of tobacco poses an enormous and distinctive threat to the public's health, being responsible for a disparate variety of lethal ailments, innumerable chronic illnesses, millions of hospital admissions, and untold human pain and suffering. This report examines in depth the current state of tobacco consumption worldwide and its increasing concentration in developing countries. It describes several aspects of tobacco consumption ... The Impact of Lifestyle Choices on Quality of Life (Qualité de Vie) and Longevity1. Introduction Although prevention of death has always been an underlying desire in man, a short but difficult life has meant that strategies aimed at achieving this end have conspicuously not been used wherein society has had a choice, since their side effects have either limited the quality of an individual's life or have resulted in death before the onset of the diseases of affluence that are now so common. However, an increased average life span has resulted from reduced starvation and the ... The Impact of Lifestyle Choices on the Quality of Health1. Introduction Good health needs care. Proper care can be taken by choosing to live a healthy lifestyle. A healthy lifestyle implies trying to remain physically active and having good habits such as physical, mental, and social well-being. A person needs to stay updated with health and to do this, he should open a library for himself where he can gather various health books, and he should also gather useful health information. This will benefit him in the long run. To live a healthy lifestyle, ... The Impact of Lifestyle Choices on General Well-being1. Introduction The impact of lifestyle choices on general well-being is significant. Many people are unaware that the simplest choices we make on a day-to-day basis can greatly affect our quality of life. Living a life full of ailments is inconvenient and can be avoided by making better lifestyle choices. One simple but significant lifestyle choice is to eat raw fruits and vegetables. Regularly consuming these foods can have a positive impact on your health and help prevent illnesses. Choosing ... The Impact of Smoking Cessation Programs on Public Health1. Introduction This research studies the impact of state smoking cessation programs on cigarette smoking both at the individual level and at the population level. A survey of 1,064 Kentuckians provides information on smoking behavior and program participation. A smoking cigarette demand estimation is carried out using the most likely participation equation. The negative effects of the measure are significant. A comparison of 2005 and 1990 datasets increases our confidence in the estimated resu ... The Impact of Lifestyle Choices on Long-Term Health Issues1. Introduction The study group on lifestyle-related diseases and the ministries of health and labour of the 195 member nations of the World Health Organization concluded that lifestyle choices contribute significantly to public health worldwide. Many of these lifestyle-related diseases limit both the number of healthy years a person lives and his or her quality of life. This paper examines lifestyle choices and the consequences of those decisions in six major issue areas: first, smoking and al ... The Effects of Smoking on Public Health and the Economy1. Introduction Smoking is a long-term addiction of younger age. It is recognized as one of the largest preventable causes of mortality, and in the prevention and reduction of smoking, it is very crucial to examine the effects of any condition and to raise awareness of the importance of the issue. In our country and worldwide, smoking prevalence is still quite high. In particular, when smoking effects are taken into consideration, the overall loss is much higher than the benefits. It is noticea ... The Impact of Addiction on Mental Health: Causes, Consequences, and Treatment Options1. Introduction Addiction and its related problems, alongside psychological complications, are widely recognized and deeply interrelated. Addicted individuals face prejudice from society and have low social acceptability. This is an area that has been widely recognized recently in the scientific environment. Among the most common addictions are alcohol, tobacco, and illicit substance use. The number of deaths due to this problem is 11.8% of the whole, and around 85.3% of all causes are related ... The Impact of Lifestyle Choices on the Prevention and Management of Chronic Diseases1. Introduction Chronic diseases have become a silent epidemic that is reaching crisis proportions because of the way people live their lives. The prevention and management of chronic diseases are heavily influenced by lifestyle choices, including physical inactivity, lack of exercise, smoking, and improper diet. Four behavioral risk factors - poor diet, physical inactivity, tobacco use, and excessive alcohol consumption - account for 60% of global deaths and almost 30% of the global burden of ... The impact of lifestyle choices on the progression of chronic kidney disease and insuficiencia renal1. Introduction High rates of chronic kidney disease (CKD) and insuficiencia renal are a concern as they silently progress, developing long-term disability, complications, and ultimately increasing the risk of death. Unhealthy lifestyle habits can lead to the development and progression of CKD, even though it is preventable and manageable with proper care and medical treatments. Clinical practice guidelines recommend risk factor modification and promote health, self-management, and shared decis ... Case Studies Using Pender's Health Promotion Model1. Introduction to Pender's Health Promotion Model Pender's Health Promotion Model (HPM) was developed to help people improve their well-being, and this model has provided useful guidance for developing health strategies in a variety of settings. Researchers have generated evidence for the efficacy and utility of the model based on modified and unmodified applications with a variety of populations and in a variety of settings. This chapter presents case studies that demonstrate the use of Pende ... Examining the Impact of Lifestyle Choices on the Prevalence of Non-Communicable Diseases in Modern Society1. Introduction Non-communicable diseases (NCDs) have become the main cause of illness and death worldwide, especially within the industrialized nations. It is predicted that by the year 2020, NCDs will contribute to up to 75% of global deaths. The increasing prevalence of these diseases is associated with societal behavioral changes, such as cigarette smoking, increased alcohol consumption, lack of physical activity, and progressive levels of obesity. Medical research has focused on the identi ... The impact of lifestyle choices on health and illness1. Introduction Though of course there are reasonable limits to the impact of subjective individual choices (smoking in enclosed public places impinging on non-smokers' health is an obvious example), nobody can seriously doubt the overall importance of individual lifestyle choices such as eating, drinking, exercise, hours of work, and sexual activity with regard to health and well-being. As in so many other areas, the fall in income poverty over time has been accompanied by a rise in depth and ... The impact of lifestyle choices on long-term health problems1. Introduction Long-term health issues plague almost everyone, but only some people are permanently beset with ailments; the remainder never appear to have health problems unless they are involved in an accident. Some of this discrepancy is related to accidents, but most long-term health problems are not caused by accidents. Health problems can arise from birth, of course, and many health problems are exacerbated by a person's living and working conditions. Yet a fundamental aspect of why some ... Teenage Smoking Essay: Writing Guide & Smoking Essay TopicsSmoking can be viewed as one of the trendy habits. Numerous teenagers try it since they think that it is cool or can help them socialize. Often students start smoking due to stress or mental illnesses. But is it okay? Educators tend to give different written assignments, which may disclose this topic. If you have to develop a teenage smoking essay, you should learn the effects and harm that this habit causes. That’s when our Custom-writing.org writers can help you!In the article, you’ll see how to deal with writing about smoking students. We’ve gathered tips for different paper types and prompts that can inspire you to start. In the end, you’ll find some smoking essay topics as well.
🔗 References✍️ how to write a teenage smoking essay. Just like any other academic paper, a teen smoking essay should be organized according to its type. You are probably familiar with the following writing ones:
Below, you can find insightful tips on how to compose a teenage smoking essay, fulfilling the requirements of each type. 🚬 Argumentative Essay on SmokingAn argumentative essay on teenage smoking should give the reader a rational discussion of a specific issue. The ideas are expected to be well-structured and solidified with valid evidence. Below, you can find the most useful tips for writing an argumentative teen smoking essay. Don’t hesitate to use them!
📈 Cause and Effect Essay on SmokingA cause and effect of the teenage smoking essay should answer two questions:
How to create an excellent cause and effect paper? You can start by checking successful teen smoking essay examples. Then, learn some useful tips here:
🚭 Persuasive Essay on SmokingA persuasive essay about teenage smoking resembles an argumentative one but has a different purpose. Here, you have to convince your reader in your opinion, using evidence and facts. Moreover, in some papers, you have to call your reader to action. For example, to quit or ban smoking . So, see how to do so:
You have a lot of ways of creating fantastic teen smoking essays. You should just turn around and gather material. Sometimes it lies near your foot. To smoke or not to smoke? – This is the question! You should decide what is for you: To be yourself or follow the fashion! It is not difficult to do! 🔥 Smoking Essay TopicsDo you know what the critical secret of a successful essay is? A well-chosen topic! If you find something you are passionate about, your essay writing process will be much easier. So, take a look at our smoking essay topics. Select one of them or use some to come up with your idea.
Teenage Smoking Essay PromptsHere are some writing prompts that you can use for your smoking essay:
Effects of Teenage Smoking Essay PromptSmoking among teenagers is a serious problem that has long-term consequences for their physical and mental health. In your essay, you can dwell on the following ideas:
Smoking in School Essay PromptDespite the implementation of smoke-free policies, a large percentage of teenagers start smoking during their school years. You can write an essay advocating for more effective initiatives to address not only students’ access to cigarettes but also the core causes of teen smoking. Check out some more ideas for your “Smoking in School” essay:
Peer Pressure Smoking Essay PromptPeer pressure is a common reason why teenagers start smoking. Friends, romantic attachments, or other social circles — all have significant effects on teens’ smoking intentions and possible tobacco addiction. Here are some practical ideas that can help you highlight the role of peer pressure in teenage smoking :
Causes of Smoking Essay PromptThere are many reasons why people start smoking, ranging from simple curiosity to complicated social and psychological factors, including anxiety, low self-esteem, and domestic violence. Check out several ideas for an essay about the causes of smoking:
Smoking Is Bad for Health Essay PromptCigarette smoking impacts nearly every organ in the body, causes a variety of diseases, and worsens smokers’ overall health. In your essay, you can expand on the following ideas to show the severe consequences of smoking on human well-being:
Is Smoking Still a Problem Among Teenagers: Argumentative Essay PromptAccording to the CDC, in 2023, 1 out of every 100 middle school students and nearly 2 out of every 100 high school students had smoked cigarettes in the past 30 days . Public health experts are especially concerned about e-cigarettes since flavorings in tobacco products can make cigarettes more appealing to teenagers. To evaluate the current situation with smoking among teens, dwell on the following ideas in your essay:
Thanks for reading till the end! Make sure to leave your opinion about the article below. Send it to your friends who may need our tips. You might also be interested in:
![essay about smoking among students Child Labor Essay: Thesis, Examples, & Writing Guide [2024]](https://custom-writing.org/blog/wp-content/uploads/2020/12/child-working-in-cambodia-e1565628499749-284x153.jpg) Children have always been apprentices and servants all over human history. However, the Industrial Revolution increased the use of child labor in the world. It became a global problem that is relevant even today when such employment is illegal. ![essay about smoking among students French Essay: Topics, Tips, and Examples [2024 Updated]](https://custom-writing.org/blog/wp-content/uploads/2020/12/french-woman-with-baguettes-street-beret-284x153.jpg) Nowadays, knowing several foreign languages is no longer surprising. For example, learning French is common for English-speaking countries. So, getting an assignment on this subject won’t be a surprise for a student.  Dissertation critique writing develops the students’ critical and logical thinking abilities. When composing, the students learn to analyze the works conducted by other researchers. To critique a dissertation, you should: In this article, we will discuss the aspects of the dissertation critique writing in detail. Our experts gathered essential tips...  So, you need to accomplish your discursive essay writing. The typical questions most students ask are: How do you write it? What is discursive essay? A discursive essay is an academic paper that involves a discussion on a particular topic. It is usually assigned to college students. You may be...  How to write a narrative essay? To do that, you need to know what a narrative essay is. It is an academic text usually written as a story and containing all the usual elements of a story. Narrative essays are often personal, experiential, and creative. Still, they should be made... ![essay about smoking among students College Essay Writing 101—the Comprehensive Guide [2024]](https://custom-writing.org/blog/wp-content/uploads/2021/01/student-girl-making-notes-in-a-copybook-with-a-pencil-e1565634333206-284x153.png) So, you can’t wait to get into college and join a fraternity, sorority, or student union. Well, we have some incredibly useful tips and helpful information for college admission essay writing! Remember: getting into college takes more than money. And outstanding essays get you great college scholarships! ![essay about smoking among students Americanism Essay: Examples, Tips & Topics [2024 Update]](https://custom-writing.org/blog/wp-content/uploads/2020/12/american-flag-284x153.jpg) It’s not hard to see why Americanism is one of the most popular essay topics. The concept of Americanism is in the center of the US identity. Writing an essay about it is an excellent way to find out more about this great country.  An art critique paper involves a comprehensive analysis and assessment of an artwork. Though this looks a bit complicated, the task doesn’t require a lot of time if you have sufficient critique writing skills. It’s an interesting assignment for students of art colleges as well as high schoolers. All you...  An article review is an academic assignment that invites you to study a piece of academic research closely. Then, you should present its summary and critically evaluate it using the knowledge you’ve gained in class and during your independent study. If you get such a task at college or university,...  Short essays answer a specific question on the subject. They usually are anywhere between 250 words and 750 words long. A paper with less than 250 words isn’t considered a finished text, so it doesn’t fall under the category of a short essay. Essays of such format are required for...  When you hear the phrase “spiritual leadership,” you probably think it’s only associated with religion. But did you know that this form of leadership can also be found in business? The book Spiritual Leadership: Moving People on to God’s Agenda by Henry and Richard Blackaby is a good starting point...  High school and college students often face challenges when crafting a compare-and-contrast essay. A well-written paper of this kind needs to be structured appropriately to earn you good grades. Knowing how to organize your ideas allows you to present your ideas in a coherent and logical manner This article by... Thank you so much this helped me a lot with an essay I had to do😁
Cigarettes smoking and e-cigarettes using among university students: a cross-section survey in Guangzhou, China, 2021
BMC Public Health volume 23 , Article number: 438 ( 2023 ) Cite this article 10k Accesses Metrics details There is an increase in the use of cigarettes and e-cigarettes worldwide, and the similar trends may be observed in young adults. Since 2014, e-cigarettes have become the most commonly used nicotine products among young adults (Sun et al., JAMA Netw Open 4:e2118788, 2021). With the increase in e-cigarette use and the decrease in use of cigarettes and other tobacco products, however, there is limited information about Chinese smokers, e-cigarettes users and trends in cigarettes and e-cigarettes use among university students. Therefore, our objective was to investigate the using status of cigarettes, e-cigarettes and smoking behavior among the students from 7 universities in Guangzhou, China. Students at 7 different universities in Guangzhou were investigated online in 2021 through a cross-sectional survey. A total of 10,008 students were recruited and after screening, 9361 participants were adopted in our statistics. Descriptive analysis, Chi-square analysis, and multiple logistic regression analysis were used to explore the smoking status and influencing factors. The average age of the 9361 university students was 22.4 years (SD = 3.6). 58.3% of participants were male. 29.8% of the participants smoked or used e-cigarettes. Among the smokers and users of e-cigarettes, 16.7% were e-cigarettes only users, 35.0% were cigarettes only users, and 48.3% were dual users. Males were more likely to smoke or use e-cigarettes. Medical students, students from prestigious Chinese universities, and students with higher levels of education were less likely. Students with unhealthy lifestyles (e.g., drinking alcohol frequently, playing video games excessively, staying up late frequently) were more likely to smoke or use e-cigarettes. Emotion can have significant impacts on both cigarettes and e-cigarettes dual users when choosing cigarettes or e-cigarettes to use. More than half of dual users said they would choose cigarettes when they were depressed and e-cigarettes when they were happy. We identified factors influencing the use of cigarettes and e-cigarettes among university students in Guangzhou, China. Gender, education level background, specialization, lifestyle habits and emotion all influenced the use of cigarettes and e-cigarettes among university students in Guangzhou, China. Male, low education level, from non-prestigious Chinese universities or vocational schools, non-medical specialization, and presence of unhealthy lifestyles were influencing factors for the use of cigarettes and e-cigarettes among university students in Guangzhou and students with these factors were more likely to smoke or use e-cigarettes. Besides, emotions can influence dual users' choice of products. This study provides more information to better understand young people's preferences for cigarettes and e-cigarettes by elucidating the characteristics of cigarettes and e-cigarettes use, as well as related influencing factors, among university students in Guangzhou. Further research involving more variables connected to the use of cigarettes and e-cigarettes will be required in our future study. Peer Review reports IntroductionDespite numerous efforts to stop the tobacco epidemic, tobacco smoking is recognized as a major preventable cause of disease worldwide [ 1 ]. The 2021 Global Report on trends in the prevalence of tobacco use 2000–2025, published by the World Health Organization (WHO), states that tobacco use in any form kills and sickens millions of people every year and over 8 million people died from a tobacco-related disease in 2019 [ 2 ]. Smoking and passive smoke (exposure to second-hand smoke) are the key contributors to the mortality of specialization chronic diseases, namely, cardiovascular disease, chronic respiratory disease, and cancer [ 3 ]. The prevalence of current (at least 1 of the last 30 days) cigarettes smoking among Chinese adults reached 27.7% in 2015, making it one of the highest smoking rates in the world [ 4 ]. The health risks of smoking have attracted more and more attention, and smoking on campus has become a serious school and social problem [ 2 , 5 ]. Customers are getting more worried about the physical harm as their awareness of cigarettes' dangers is increased, and they are more encouraged to choose e-cigarettes which are claimed as less harmful and can meet their needs of risk reduction [ 6 ]. Many researches have shown that e-cigarettes, although they cannot be considered safe [ 7 ], may cause less harm to the body than cigarettes [ 8 , 9 , 10 , 11 ]. Some cigarettes smokers are converting to e-cigarettes to avoid the effects of smoking [ 12 ]. E-cigarettes are electronic devices that deliver nicotine to the respiratory system by atomizing an aerosol of smoke containing glycerin, propylene glycol, nicotine and other additives through an electric heating element [ 13 ]. Since e-cigarettes produce much less tar, carbon monoxide, and carcinogenic ingredients such as aldehydes, acids, and phenols, the exclusive use of e-cigarettes among smokers may reduce the number of diseases caused by such ingredients [ 14 , 15 , 16 ]. Studies have shown that cigarettes and e-cigarettes are the most frequently used nicotine products in youth adults in the USA [ 17 , 18 , 19 , 20 ] and probably China. China is the world’s largest consumer of tobacco products and contributes substantially to the global burden of smoking-related diseases [ 21 ]. It is noteworthy that the use of e-cigarettes in China is far less frequent than in some European countries and the United States [ 22 , 21 , 22 , 23 , 24 , 27 ]. However, the health risks of e-cigarettes have not been adequately studied, data on their effects and risks on human body are limited [ 15 , 28 ]. Despite the fact that using e-cigarettes is a worldwide phenomenon [ 29 , 30 ], there is a paucity of data regarding the knowledge and attitude of e-cigarettes users particularly among the young adults in China [ 31 ]. Studies of cigarettes and e-cigarettes use among e-cigarettes consumers are still in their infancy, with most of them being questionnaires about basic consumer information, consumption behavior and preferences. Most survey respondents are European and American e-cigarettes consumers, and there are limited reports on Chinese e-cigarettes consumers' vaping behavior. There is an urgent need to investigate the status quo and influence factors of smoking and using e-cigarettes [ 32 ]. Therefore, we conducted a cross-sectional survey of using cigarettes and e-cigarettes to investigate the smoking behaviors among university students in Guangzhou. One of our research interests was the use of cigarettes and e-cigarettes among university students. Another focus was on the factors that influence the use of cigarettes and e-cigarettes by university students. Research design and participantsA cross-sectional survey was developed in China that collected data through a self-administered online structured questionnaire from July to December 2021 among undergraduate and graduate students with different disciplinary backgrounds from 7 universities in Guangzhou. In total, 10,008 participants were recruited through WeChat, while 9361 university students completed the questionnaire with a response rate of 93.5%. The online survey was anonymous, and data were encrypted for added security protection. Before entering the online survey system, all participants reviewed and approved the electronic consent page. By prohibiting users with the same IP (Internet Protocol) address from accessing the survey more than once, duplicate entries were avoided. Incomplete surveys were not sent to the system because of a missed response reminder component that alerted participants in real time about incomplete surveys. This investigation was conducted after obtaining the approval of the Ethics Review Committee (IRB), whose approval number is SYSU202108001. SociodemographicParticipants self-reported their gender, age, race/ethnicity, levels of education, and monthly living expenses. We also distinguished the university by three types (vocational school, general universities and prestigious universities) including 7 different universities in Guangzhou, China. A separate variable was created to distinguish the specialization of participants (medical specialization or not). Cigarettes and e-cigarettes useRespondents to the survey were asked whether they had smoked or used e-cigarettes even once. Those who had ever smoked or used e-cigarettes were asked if they now smoke or use e-cigarettes. We defined current cigarettes or(and) e-cigarettes use as having smoked or(and) used e-cigarettes at least one day in the last 30 days. Current cigarettes or(and) e-cigarettes users were asked about the age at first use of cigarettes or e-cigarettes and the product of choice for first use (cigarettes or e-cigarettes). Respondents also were asked how long they have been smoking or using e-cigarettes with the possible answers being from within a month to more than ten years. The using product of initiation (cigarettes or e-cigarettes) was asked if the respondent was a dual user. Regarding the future choices of smokers and e-cigarettes users, the main focus was to examine whether they choose to become cigarettes only users, e-cigarettes only users or dual users in a year. Lifestyles variablesPrevious studies [ 17 , 18 , 33 ] have shown that unhealthy lifestyles such as alcohol abuse, video gaming addiction, and sleep deprivation are strongly associated with smoking or using e-cigarettes in young adults, so we added lifestyle variables to the study. Three common unhealthy lifestyles were distinguished in our questionnaire including drinking alcohol excessively, playing video games frequently and staying up late (falling asleep after 24 o’clock and getting tired next morning) frequently. We defined frequently as more than three times in a week, and excessively as play video games more than 20 h per week. Related concepts and definitionsIn the survey, participants were divided into four types: cigarettes only users (cigarettes smokers who currently do not use e-cigarettes), e-cigarettes only users (e-cigarettes users who currently do not use cigarettes), dual users (those who currently use both cigarettes and e-cigarettes) and non-nicotine users (those who currently do not use cigarettes and e-cigarettes). The selected Chinese universities were classified according to their academic prominence as prestigious and non-prestigious according to the QS World University Rankings [ 34 ]. Prestigious Chinese universities refer to Sun Yat-sen University and Jinan University in this study. Non-prestigious Chinese universities include Guangzhou University of Chinese Medicine, Southern Medical University and Guangzhou City Polytechnic. Guangzhou Institute of Science and Technology and Guangzhou Huashang University are vocational schools in China. Statistical analysisThe categorical variables were expressed as the frequency (%), while the continuous variables were presented as mean ± SD. A single sample Kolmogorov–Smirnov test was used to test whether the data conform to normal distribution. Chi square test was used to compare categorical variables, while independent sample t-test and Mann–whitney U test were respectively used to compare the continuous variables with and without normal distribution. An analysis of multiple logistic regression was conducted to explore the relationship between using behavior of cigarettes and e-cigarettes and lifestyle. When multiple comparisons were involved, the Bonferroni method was used to correct for the test level α. All analyses were done using R software. Significant test was a bilateral test and the level of statistical significance was set at P < 0.05 for all the analyses. Participant characteristics and status of cigarettes and e-cigarettes useTable 1 shows characteristics of participants. The final sample was composed of 9361 individuals, providing a response rate of 93.5%. In the full sample of 9361 participants, 58.3% ( n = 5461) were male and 41.7% ( n = 3900) were female. Table 1 shows that 29.8% of students smoke or use e-cigarettes and that among them, the typical patterns is dual use (48.3%) with 35.0% smoking only cigarettes and 16.7% using only e-cigarettes. Among the dual users, 51.2% ( n = 690) participants started using cigarettes, 34.4% ( n = 464) participants e-cigarettes, 14.4% ( n = 193) did not recall the exact order (Fig. 1 ). 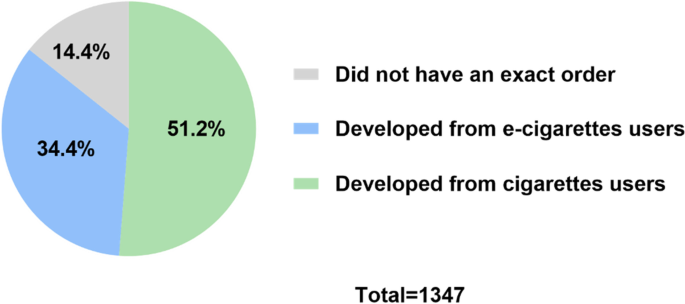 The source distribution of cigarettes and e-cigarettes dual users among university students in Guangzhou, China Factors associated with smoking or using e-cigarettesTable 2 shows factors associated with smoking or using e-cigarettes. Among e-cigarettes users, females were more likely to choose e-cigarettes compared to males (78.1 vs. 62.8%, P < 0.05). In general, medical students have a higher level of knowledges about health [ 16 , 35 ] and it is important to understand their perceptions of e-cigarettes as they need to communicate and interact with patients during their training and later in their careers. Therefore, we divided the specialization into non-medical specialization and medical specialization, using medicine as a criterion. The prevalence of cigarettes and e-cigarettes was significantly higher among non-medical specialization than medical specialization (32.7% vs. 12.8%, P < 0.05), and the highest rate of cigarettes and e-cigarettes use was found among law specialization compared to medical specialization (47.2% vs. 12.8%, P < 0.05), followed by history (46.1% vs. 12.8%) and philosophy (43.8% vs. 12.8%, P < 0.05).However, there was no difference in the choice of cigarettes or e-cigarettes between non-medical and medical students. The use of both e-cigarettes and cigarettes was lower in prestigious Chinese universities compared to other types of schools. Students in non-prestigious Chinese universities had the highest rate of cigarettes and e-cigarettes use and a correspondingly higher rate of e-cigarettes use. Among the participants, undergraduates and vocational school students had the highest rate of cigarettes and e-cigarettes use (32.8% and 31.8%), followed by Ph.D. students (20.2%), while master students had the lowest rate of cigarettes and e-cigarettes use at 9.7%, with a statistically significant difference ( P < 0.05). Among them, there was no difference in the distribution of cigarettes and e-cigarettes use among undergraduates and vocational school students, while the rate of cigarettes use among master students was significantly lower than other students ( P < 0.05), and the rate of e-cigarettes use? was also the lowest. Lifestyles have significant impacts on the use of cigarettes and e-cigarettes. Compared to those with appropriate lifestyles, students who drank alcohol frequently, played video games excessively, stayed up late frequently, and did all of the above had an increased odds of cigarettes use, e-cigarettes use, and dual use. Multiple logistic regression analyses of cigarettes only users, e-cigarettes only users, and dual users indicated that the using of cigarettes, e-cigarettes and dual use increased 8.1, 6.8 and 10.2 times respectively for those who drank alcohol compared to those who did not drink alcohol; The odds of cigarettes using, e-cigarettes using and dual using were 2.6, 3.2, and 4.7 times higher for gamers compared to non-gamers, respectively; The odds of cigarettes using, e-cigarettes using and dual using increased by 1.3, 1.2 and 2.4 times respectively for those who stayed up late compared to those who did not stay up late. All results are presented in Table 3 . Table 4 shows that 83.5% ( n = 1125) of dual users chose using products (whether cigarettes or e-cigarettes) according to their emotional state, while 56.5% ( n = 761) of dual users chose cigarettes when they are depressed and e-cigarettes when they are happy. Future choices of smokers and e-cigarettes usersTable 5 shows that e-cigarettes only users and dual users have a stronger intention to quit using their current nicotine product of use than cigarettes only users( P < 0.05). Figure 2 displays the willingness of cigarettes only users or e-cigarettes only users to try another product (cigarettes or e-cigarettes) among university students in Guangzhou, China. For cigarettes only users, 41.8% ( n = 408) report that they will not use e-cigarettes in the future, 30.9% ( n = 301) use both cigarettes and e-cigarettes in the future, and 27.3% ( n = 266) would give up cigarettes and use e-cigarettes. For e-cigarettes only users, 42.0% ( n = 195) would give up e-cigarettes and only use cigarettes, 37.5% ( n = 174) would use both cigarettes and e-cigarettes, and 20.5% ( n = 95) would not use cigarettes in the future. 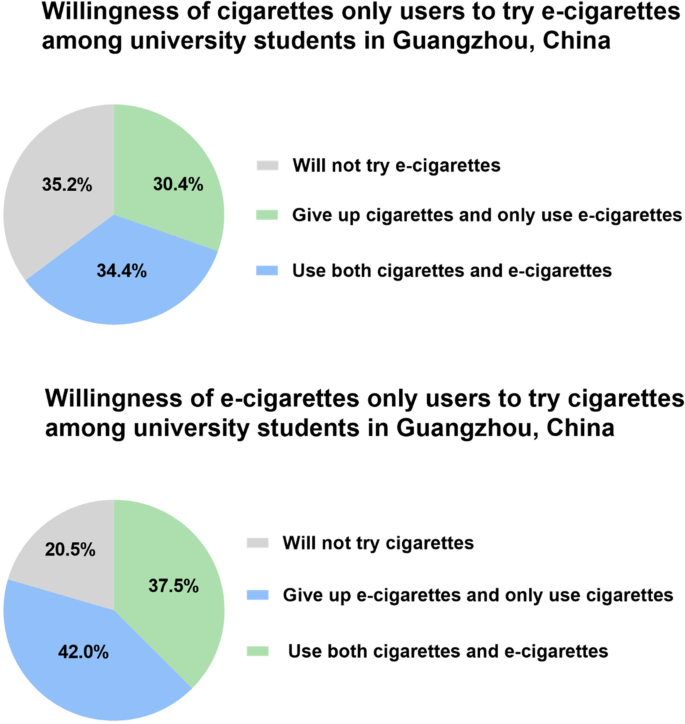 Willingness of cigarettes only users or e-cigarettes only users to try another nicotine product among university students in Guangzhou, China Our findings were consistent with some prior prevalence studies in which males were more likely to smoke than females (males: females = 37.2:7.5) [ 10 , 36 , 35 , 38 ]. However, the gender difference in e-cigarettes were smaller than in cigarettes, which is also consistent with previous research studies [ 39 , 38 , 41 ]. The gender differences in smoking may be attributed to traditional sociocultural influences [ 31 , 32 , 42 , 41 , 44 ]. Habitual thinking suggests that female's smoking is associated with an inappropriate social image. The social circumstances put more pressure on female smokers, whereas, for male smokers, social opinion has a much smaller negative impact than for females, suggesting that the socio-cultural context have an intervening role in smoking. In addition, we found that the rate of using cigarettes and e-cigarettes was the highest among undergraduates, followed by Ph.D. students, and the lowest was among master students, both for cigarettes, e-cigarettes, and dual use. It indicates that cigarettes and e-cigarettes use was shown as a non-linear relationship with education level, which is consistent with other studies [ 45 ]. This may be due to the fact that undergraduates have less academic stress and more social activities [ 46 ], which are susceptibility factors for cigarettes and e-cigarettes use. A number of studies have shown that there is a significant correlation between smoking and the education level of the smoker, the higher the education level is, the lower the smoking rate is [ 47 , 48 ]. This is because people with a higher level of education level have a higher level of health awareness, and a relatively higher level of awareness of the diseases caused by smoking and harmful results [ 49 , 50 ], and thus have a lower smoking rate, which explains the relatively lower rate of cigarettes and e-cigarettes use among master student s and Ph.D. students. Undergraduate students were more likely to use e-cigarettes, in contrast to master students and Ph.D. students, who had the lowest rates of cigarettes and e-cigarettes use and a greater preference for cigarettes. It has been established that e-cigarettes use shows a non-linear relationship with education level, but the exact reasons for this are unclear and warrant further study [ 51 ]. Our findings displayed that the use of both e-cigarettes and cigarettes was lower in prestigious Chinese universities perhaps due to the widely different circumstances, different management, and different type of student in different universities. In addition, we found that the cigarettes use rate of Ph.D. students is much higher than the e-cigarettes use rate, which is different from the situation of undergraduates and vocational school students. The reasons for this may be that Ph.D. students are older than others and e-cigarettes are emerging products, so many Ph.D. students are used to using cigarettes and are not familiar or are not willing to try e-cigarettes. Similar to previous surveys, we found that non-medical students have higher rates of cigarettes and e-cigarettes use than medical students [ 52 ]. This may be due to the fact that medical students are more aware of the effects of nicotine on the body after learning extensive knowledge of physiology and pathology [ 16 , 30 , 43 ]. It is noteworthy that, the highest rate of using cigarettes and e-cigarettes was law students. The considerable pressure placed on them in academic performance can explain this result [ 53 ]. A growing body of research indicates that emotion is also one of the influencing factors of smoking and negative emotions can induce smoking [ 54 , 55 ]. Our findings found that the majority of dual users will use cigarettes rather than e-cigarettes when they are depressed. This result may be due to the different experiences of smoking and vaping while there is no related data to illustrate that smoking cigarettes will provide more pleasure in the present. We also discovered that among all the future choices, dual use is becoming increasingly popular, as the previous study reported [ 56 ]. 51.2% of the dual users started as cigarettes only users, indicating a huge shift of nicotine products using pattern in young adults. Consistent with our findings above, some studies [ 30 , 41 , 57 ] also indicated that cigarettes only users are more likely to try e-cigarettes than non-smokers. However, a study by Sean Esteban McCabe et al. indicated that dual users had the greatest risk for engaging in risk behaviors (including truancy, grade point average < = C + , binge drinking, alcohol use, marijuana use, illicit drug use and nonmedical Rx drug use) followed by cigarettes only users, e-cigarettes only users, and non-nicotine products users [ 5 ]. LimitationsThere are several limitations to this study. First, the source of the sample was university students, whose smoking behaviors may differ from the general population of young adults and may not apply to the group who are not students. Second, the data was not weighted for adjusting biases to non-equal probability of selection, non-coverage, and non-response. Third, these data are self-reported and might be subject to reporting bias. Finally, the study was a cross-sectional study and could not dynamically observe changes in cigarette and e-cigarette use, we were unable to assess causal relationships. The present study reveals the use rate of cigarettes and e-cigarettes among university students in Guangzhou, China. This study also provides the possible future choices of cigarettes or e-cigarettes users among university students. Our investigation shows that 29.8% of participants reports that they used cigarettes or e-cigarettes. Among them, 16.7% were e-cigarettes only users, 35.0% were cigarettes only users and 48.3%were dual users. 51.2% of the dual users were developed from cigarette only users. Additionally, this study investigated influencing factors to cigarettes and e-cigarettes use, showing that gender, school, education level, specialization, and lifestyles all had impacts on the use of cigarettes and e-cigarettes among university students in Guangzhou. Students who were male, had low education levels, from non-prestigious Chinese universities or vocational schools, had non-medical specialization, and the presence of inappropriate lifestyles such as drinking and playing video games excessively were more likely to use cigarettes and e-cigarettes. Besides, emotion also can have significant effects on the choice of using cigarettes or e-cigarettes for dual users. This study elucidates the characteristics of cigarettes and e-cigarettes use and related influencing factors among university students in Guangzhou, providing more information to better understand young people's preferences for cigarettes and e-cigarettes. This cross-section survey offers a perspective for policy makers to develop more guiding industry rules of young adult's cigarettes and e-cigarettes using. In our future work, further investigations, which take more variables related to cigarettes and e-cigarettes using into account, will need to be undertaken, and more reliable analytical methods must be required. Availability of data and materialsAll data generated or analyzed during this study are included in this published article. Perez-Warnisher MT, Carballosa de Miguel MDP, Seijo LM. Tobacco Use Worldwide: legislative efforts to curb consumption. Ann Glob Health. 2019;85(1). WHO global report on trends in prevalence of tobacco use 2000–2025, fourth edition [ https://www.who.int/publications-detail-redirect/9789240039322 ]. Xie B, Palmer P, Li Y, Lin C, Johnson CA. Developmental trajectories of cigarette use and associations with multilayered risk factors among Chinese adolescents. Nicotine Tob Res. 2013;15(10):1673–81. Article PubMed PubMed Central Google Scholar Goodchild M, Zheng R. Tobacco control and Healthy China 2030. Tob Control. 2019;28(4):409–13. Article PubMed Google Scholar McCabe SE, West BT, Veliz P, Boyd CJ. E-cigarette use, cigarette smoking, dual use, and problem behaviors among U.S. Adolescents: results from a national survey. J Adolesc Health. 2017;61(2):155–62. Wang L, Wang Y, Chen J, Yang XM, Jiang XT, Liu P, Li M. Comparison of biological and transcriptomic effects of conventional cigarette and electronic cigarette smoke exposure at toxicological dose in BEAS-2B cells. Ecotoxicol Environ Saf. 2021;222:112472. Article CAS PubMed Google Scholar Sharan RN, Chanu TM, Chakrabarty TK, Farsalinos K. Patterns of tobacco and e-cigarette use status in India: a cross-sectional survey of 3000 vapers in eight Indian cities. Harm Reduct J. 2020;17(1):21. Tavolacci MP, Vasiliu A, Romo L, Kotbagi G, Kern L, Ladner J. Patterns of electronic cigarette use in current and ever users among college students in France: a cross-sectional study. BMJ Open. 2016;6(5):e011344. Pisinger C, Dossing M. A systematic review of health effects of electronic cigarettes. Prev Med. 2014;69:248–60. Alzalabani AA, Eltaher SM. Perceptions and reasons of E-cigarette use among medical students: an internet-based survey. J Egypt Public Health Assoc. 2020;95(1):21. Barbeau AM, Burda J, Siegel M. Perceived efficacy of e-cigarettes versus nicotine replacement therapy among successful e-cigarette users: a qualitative approach. Addict Sci Clin Pract. 2013;8(1):5. Pasquereau A, Guignard R, Andler R, Nguyen-Thanh V. Electronic cigarettes, quit attempts and smoking cessation: a 6-month follow-up. Addiction. 2017;112(9):1620–8. Kinouani S, Pereira E, Tzourio C. Electronic cigarette use in students and its relation with tobacco-smoking: a cross-sectional analysis of the i-share study. Int J Environ Res Public Health. 2017;14(11):1345. Go YY, Mun JY, Chae SW, Chang J, Song JJ. Comparison between in vitro toxicities of tobacco- and menthol-flavored electronic cigarette liquids on human middle ear epithelial cells. Sci Rep. 2020;10(1):2544. Article CAS PubMed PubMed Central Google Scholar Schraufnagel DE, Blasi F, Drummond MB, Lam DC, Latif E, Rosen MJ, Sansores R, Van Zyl-Smit R. Forum of International Respiratory S: Electronic cigarettes. A position statement of the forum of international respiratory societies. Am J Respir Crit Care Med. 2014;190(6):611–8. Al-Sawalha NA, Almomani BA, Mokhemer E, Al-Shatnawi SF, Bdeir R. E-cigarettes use among university students in Jordan: Perception and related knowledge. PLoS ONE. 2021;16(12):e0262090. Raiff BR, Jarvis BP, Rapoza D. Prevalence of Video Game Use, Cigarette Smoking, and Acceptability of a Video Game-Based Smoking Cessation Intervention Among Online Adults. Nicotine Tob Res. 2012;14(12):1453–7. Hughes K, Bellis MA, Hardcastle KA, McHale P, Bennett A, Ireland R, Pike K. Associations between e-cigarette access and smoking and drinking behaviours in teenagers. BMC Public Health. 2015;15(1):244. Sun R, Mendez D, Warner KE. Trends in Nicotine Product Use Among US Adolescents, 1999–2020. JAMA Netw Open. 2021;4(8):e2118788. Gotts JE, Jordt SE, McConnell R, Tarran R. What are the respiratory effects of e-cigarettes? BMJ. 2019;366:l5275. Zheng Y, Ji Y, Dong H, Chang C. The prevalence of smoking, second-hand smoke exposure, and knowledge of the health hazards of smoking among internal migrants in 12 provinces in China: a cross-sectional analysis. BMC Public Health. 2018;18(1):655. Copeland AL, Peltier MR, Waldo K. Perceived risk and benefits of e-cigarette use among college students. Addict Behav. 2017;71:31–7. Lanza HI, Teeter H. Electronic Nicotine Delivery Systems (E-cigarette/Vape) use and Co-occurring health-risk behaviors among an ethnically diverse sample of young adults. Subst Use Misuse. 2018;53(1):154–61. Delnevo CD, Giovenco DP, Steinberg MB, Villanti AC, Pearson JL, Niaura RS, Abrams DB. Patterns of Electronic Cigarette Use Among Adults in the United States. Nicotine Tob Res. 2016;18(5):715–9. Wallace LN, Roche MJ. Vaping in Context: Links Among E-cigarette Use, Social Status, and Peer Influence for College Students. J Drug Educ. 2018;48(1–2):36–53. Article Google Scholar Grant JE, Lust K, Fridberg DJ, King AC, Chamberlain SR. E-cigarette use (vaping) is associated with illicit drug use, mental health problems, and impulsivity in university students. Ann Clin Psychiatry. 2019;31(1):27–35. Jones RD, Asare M, Lanning B. A Retrospective Cross-Sectional Study on the Prevalence of E-cigarette Use Among College Students. J Community Health. 2021;46(1):195–202. Gorna I, Napierala M, Florek E: Electronic Cigarette Use and Metabolic Syndrome Development: A Critical Review. Toxics 2020, 8(4). Misra M, Leverette RD, Cooper BT, Bennett MB, Brown SE. Comparative in vitro toxicity profile of electronic and tobacco cigarettes, smokeless tobacco and nicotine replacement therapy products: e-liquids, extracts and collected aerosols. Int J Environ Res Public Health. 2014;11(11):11325–47. Iqbal N, Khan ZA, Anwar SMH, Irfan O, Irfan B, Mushtaq A, Bibi M, Siddiqui F, Khan JA. Electronic cigarettes use and perception amongst medical students: a cross sectional survey from Sindh, Pakistan. BMC Res Notes. 2018;11(1):188. Mao R, Li X, Stanton B, Wang J, Hong Y, Zhang H, Chen X. Psychosocial correlates of cigarette smoking among college students in China. Health Educ Res. 2009;24(1):105–18. Eticha T, Kidane F. The prevalence of and factors associated with current smoking among College of Health Sciences students, Mekelle University in northern Ethiopia. PLoS ONE. 2014;9(10):e111033. Wetter DW, Young TB. The relation between cigarette smoking and sleep disturbance. Prev Med. 1994;23(3):328–34. QS World University Rankings 2021 [ https://www.topuniversities.com/university-rankings/world-university-rankings/2021 ]. Alenazi ASABAAMSMAKAFAAAOT. Knowledge and attitudes toward HIV among medical and non-medical students in Riyadh, Saudi Arabia. Int J Med Dev Countries. 2020;4(12):2120–30. Google Scholar Bin Abdulrahman KA, Khalaf AM, Bin Abbas FB, Alanezi OT. The lifestyle of Saudi medical students. Int J Environ Res Public Health. 2021;18(15):7869. Kong G, Idrisov B, Galimov A, Masagutov R, Sussman S. Electronic Cigarette Use Among Adolescents in the Russian Federation. Subst Use Misuse. 2017;52(3):332–9. Bhaskar RK, Sah MN, Gaurav K, Bhaskar SC, Singh R, Yadav MK, Ojha S. Prevalence and correlates of tobacco use among adolescents in the schools of Kalaiya, Nepal: a cross-sectional questionnaire based study. Tob Induc Dis. 2016;14:11. Zhu J, Shi F, Xu G, Li N, Li J, He Y, Yu J. Conventional Cigarette and E-Cigarette Smoking among School Personnel in Shanghai, China: Prevalence and Determinants. Int J Environ Res Public Health. 2019;16(17):3197. Brozek GM, Jankowski M, Lawson JA, Shpakou A, Poznanski M, Zielonka TM, Klimatckaia L, Loginovich Y, Rachel M, Gereova J, et al. The prevalence of cigarette and e-cigarette smoking among students in central and eastern europe-results of the YUPESS study. Int J Environ Res Public Health. 2019;16(13):2297. Balogh E, Wagner Z, Faubl N, Riemenschneider H, Voigt K, Terebessy A, Horvath F, Fuzesi Z, Kiss I. Increasing prevalence of electronic cigarette use among medical students. repeated cross-sectional multicenter surveys in Germany and hungary, 2016-2018. Subst Use Misuse. 2020;55(13):2109–15. MbatchouNgahane BH, Luma H, Mapoure YN, Fotso ZM, AfaneZe E. Correlates of cigarette smoking among university students in Cameroon. Int J Tuberc Lung Dis. 2013;17(2):270–4. Article CAS Google Scholar Khader YS, Alsadi AA. Smoking habits among university students in Jordan: prevalence and associated factors. East Mediterr Health J. 2008;14(4):897–904. CAS PubMed Google Scholar Prijic Z, Igic R. Cigarette smoking and medical students. J BUON. 2021;26(5):1709–18. PubMed Google Scholar Assari S, Mistry R, Bazargan M. Race, educational attainment, and e-cigarette use. J Med Res Innov. 2020;4(1). https://doi.org/10.32892/jmri.185 . Martin LM, Sayette MA. A review of the effects of nicotine on social functioning. Exp Clin Psychopharmacol. 2018;26(5):425–39. Shuja M, Sarrafzadegan N, Roohafza HR, Sadeghi M, Ghafari M, Mohammadian M, MohammadianHafshejani A. Factors associated with cigarette smoking in central parts of Iran. Asian Pac J Cancer Prev. 2017;18(3):647–53. PubMed PubMed Central Google Scholar Böckerman P, Hyytinen A, Kaprio J. Smoking and long-term labour market outcomes. Tob Control. 2015;24(4):348–53. van der Heide I, Wang J, Droomers M, Spreeuwenberg P, Rademakers J, Uiters E. The relationship between health, education, and health literacy: results from the Dutch Adult Literacy and Life Skills Survey. J Health Commun. 2013;18(Suppl 1):172–84. Sudhakar S, Aebi ME, Burant CJ, Wilson B, Wenk J, Briggs FBS, Pyatka N, Blixen C, Sajatovic M. Health literacy and education level correlates of participation and outcome in a remotely delivered epilepsy self-management program. Epilepsy Behav. 2020;107:107026. Wilson FA, Wang Y. Recent Findings on the Prevalence of E-Cigarette Use Among Adults in the U.S. Am J Prev Med. 2017;52(3):385–90. Hinderaker K, Power DV, Allen S, Parker E, Okuyemi K. What do medical students know about e-cigarettes? A cross-sectional survey from one U.S. medical school. BMC Med Educ. 2018;18(1):32. Bergin A, Pakenham K. Law Student Stress: Relationships Between Academic Demands, Social Isolation, Career Pressure, Study/Life Imbalance and Adjustment Outcomes in Law Students. Psychiatry, Psychology and Law. 2015;22(3):388–406. Weinberger AH, McKee SA. Mood and smoking behavior: the role of expectancy accessibility and gender. Addict Behav. 2012;37(12):1349–52. Weinberger AH, McKee SA. Gender differences in smoking following an implicit mood induction. Nicotine Tob Res. 2012;14(5):621–5. Lee S, Grana RA, Glantz SA. Electronic cigarette use among Korean adolescents: a cross-sectional study of market penetration, dual use, and relationship to quit attempts and former smoking. J Adolesc Health. 2014;54(6):684–90. Bowker K, Lewis S, Phillips L, Orton S, Ussher M, Naughton F, Bauld L, Coleman T, Sinclair L, McRobbie H, et al. Pregnant women’s use of e-cigarettes in the UK: a cross-sectional survey. BJOG. 2021;128(6):984–93. Download references AcknowledgementsNot applicable. Informed consent was obtained from all subjects. Informed consent was obtained from all subjects and/or their legal guardian(s). This work was supported by the National Natural Science Foundation of China (31970699), the Guangdong Basic and Applied Basic Research Foundation (2021A1515010766 and 2019A1515011030), the Guang-dong Provincial Key Laboratory of Construction Foundation(2019B030301005), the Key-Area Research and Development Program of Guangdong Province (2020B1111110003), and the National Major Special Projects for the Creation and Manufacture of New Drugs(2019ZX09301104). Author informationAuthors and affiliations. Department of Pharmacology and Toxicology, School of Pharmaceutical Sciences, Sun Yat-Sen University, Guangzhou, 510006, Guangdong, China Hongjia Song, Wanchun Yang, Yuxing Dai, Guangye Huang, Min Li, Guoping Zhong, Peiqing Liu & Jianwen Chen School of Pharmaceutical Sciences, National and Local Joint Engineering Laboratory of Druggability and New Drugs Evaluation, Guangdong Engineering Laboratoty of Druggability and New Drug Evaluation, School of Pharmaceutical Sciences, Sun Yat-Sen University, Guangzhou, 510006, PR China RELX Lab, Shenzhen RELX Tech. Co, Ltd., Shenzhen, 518000, Guangdong, China Xuemin Yang, Kun Duan & Xingtao Jiang You can also search for this author in PubMed Google Scholar ContributionsPL and JC contributed to the conception of the study. XY and HS participated in designing the research, performing the bibliography searches, selecting studies and extracting data. WY and HS contributed significantly to analysis and manuscript preparation. HS performed the data analyses and wrote the manuscript. YD, GZ and HS contributed to the interpretation and discussion of the results of the analysis. All authors edited and critically reviewed the manuscript. All authors read and approved the final manuscript. Corresponding authorsCorrespondence to Guoping Zhong , Peiqing Liu or Jianwen Chen . Ethics declarationsEthical approval and consent to participate.. Students from universities and vocational schools in Guangzhou, China received an online survey after their consent. Ethical approval was obtained from Dongguan Kanghua Hospital Clinical Trial Research Ethics Committee (Approval number: SYSU202108001). This study was conducted in accordance with the Declaration of Helsinki. All methods were performed in accordance with the relevant guidelines and regulations. Consent for publicationCompeting interests. At the time of the research, Xuemin Yang, Kun Duan and Xingtao Jiang were employees of RELX Tech. The rest of the authors have no competing interests to disclose. Additional informationPublisher’s note. Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Rights and permissionsOpen Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data. Reprints and permissions About this articleCite this article. Song, H., Yang, X., Yang, W. et al. Cigarettes smoking and e-cigarettes using among university students: a cross-section survey in Guangzhou, China, 2021. BMC Public Health 23 , 438 (2023). https://doi.org/10.1186/s12889-023-15350-2 Download citation Received : 20 August 2022 Accepted : 28 February 2023 Published : 07 March 2023 DOI : https://doi.org/10.1186/s12889-023-15350-2 Share this articleAnyone you share the following link with will be able to read this content: Sorry, a shareable link is not currently available for this article. Provided by the Springer Nature SharedIt content-sharing initiative
BMC Public HealthISSN: 1471-2458
Personal and social factors as a determinate of adolescent smoking
21 ReferencesAn investigation of family factors that predict smoking among high school adolescents, a qualitative research on the problems and expectations of imam hatip secondary school students (the case of istanbul province), effects of smoking ban in turkey on patients with chronic obstructive pulmonary disease: a retrospective analysis, mesleki̇ ve tekni̇k anadolu li̇sesi̇ algisi: ortaokul 8. sinif öğrenci̇leri̇ üzeri̇ne bi̇r araştirma, tobacco taxation in turkey : an overview of policy measures and results, parents’ and peers’ normative influence on adolescents’ smoking: results from a swiss-italian sample of middle schools students, lise öğrencileri arasında sigara, alkol kullanım sıklığı ve etkileyen faktörler, association between family and friend smoking status and adolescent smoking behavior and e-cigarette use in korea, the association between peer, parental influence and tobacco product features and earlier age of onset of regular smoking among adults in 27 european countries., adolescents’ perceptions of light and intermittent smoking in the united states, related papers. Showing 1 through 3 of 0 Related Papers
Factors Related to Smoking Habits of Male Adolescents
Tobacco Induced Diseases volume 2 , Article number: 133 ( 2004 ) Cite this article 31k Accesses 21 Citations Metrics details A cross-sectional study was conducted to identify the factors related to smoking habits of adolescents among secondary school boys in Kelantan state, Malaysia. A total of 451 upper secondary male students from day, boarding and vocational schools were investigated using a structured questionnaire. Cluster sampling was applied to achieve the required sample size. The significant findings included: 1) the highest prevalence of smoking was found among schoolboys from the vocational school; 2) mean duration of smoking was 2.5 years; 3) there were significant associations between smoking status and parents' smoking history, academic performance, perception of the health hazards of smoking, and type of school attended. Peer influence was the major reason students gave for taking up the habit. Religion was most often indicated by non-smokers as their reason for not smoking. Approximately 3/5 of the smokers had considered quitting and 45% of them had tried at least once to stop smoking. Mass media was indicated as the best information source for the students to acquire knowledge about negative aspects of the smoking habit. The authors believe an epidemic of tobacco use is imminent if drastic action is not taken, and recommend that anti-smoking campaigns with an emphasis on the religious aspect should start as early as in primary school. Intervention programs to encourage behavior modification of adolescents are also recommended. IntroductionSmoking is the single most important preventable cause of death [ 1 ]. The secondary school age is a critical period in the formation of the smoking habit. Most smokers start smoking during their adolescence or early adult years. The earlier they start to smoke, the more likely they are to become regular smokers [ 2 , 3 ]. Those concerned about the health, welfare and education of young people should be anxious to find ways to prevent them from taking up this habit. In Malaysia, with the improvement of socioeconomic status and the standard of health care, the incidence of communicable diseases has declined significantly, but other health problems are emerging. An example of the diseases related to smoking is coronary artery disease, which now is the main cause of death in hospitals in peninsular Malaysia [ 4 ]. Adolescent and teenage smoking have been studied widely, and it has been found in developed countries that nearly one-half of school students who have reached the age of 18 have already established the habit of smoking with some degree of regularity, and it is a rather unrealistic hope on the part of adults to expect that children will abstain until reaching the adult approved age of decision [ 5 ]. Smoking is a major problem among youth in Malaysia. In a recent survey by the Ministry of Youth and Sports on negative behaviors among 5,860 adolescents, 80% indicated that they had ever experienced smoking [ 6 ]. Schooling is the major activity of most children between the ages of 7 and 17 years and school is the place where most of them socialize outside their home environment for the first time. A school is the place where much knowledge is obtained, attitudes are formed and sometimes habits are chosen. Studies have demonstrated that the secondary school age is a critical period in the formation of the smoking habit [ 7 ]. Experimenting with cigarettes often begins during childhood or early adolescence and there is usually a period of about 1.5 to 2 years between initiation of smoking and establishment of the smoking habit [ 8 , 9 ]. Schooling is compulsory in Malaysia. A child enters school at the age of 7 and attends primary school for six years, after which he enters lower secondary school (Form I–III). At the end of Form III there is a qualifying examination, and only students who pass this examination proceed to upper secondary school (Form IV–V). Those who fail repeat Form III, go to vocational or private schools, or drop out of school [ 10 ]. A number of factors influence an individual to start smoking. Lack of awareness and knowledge have been reported as contributing factors based on studies in the past. This study aimed to highlight environmental, religious and other factors influencing smoking in male adolescents in secondary schools. A cross-sectional study was conducted during January through June 2001. Applying the cluster sampling method, 451 Form IV and V (upper secondary) male students from three different schools (day, boarding and vocational) were included in the study. The reason for selecting different schools was to examine smoking habits in relation to the nature of the schools attended by the students. Only male adolescents were included in the study. The number of participants from each school were: 150 from day school (33.26%), 150 from boarding school (33.26%) and 151 from vocational school (33.48%). Since the population of Kelantan state is 90% Islamic, all study participants were Malay Muslim schoolboys. A structured questionnaire was distributed among them for self-administration with prior explanation. Subjects were asked to indicate their reasons for smoking or non-smoking based on factors such as religion, parental control, parental smoking status, peer influence, feeling of maturity, enjoyment, monetary and other factors. The validity and reliability of the questionnaire was tested earlier based on pre-test results, using statistical software. Smoking status was self-reported, and was not verified by any biochemical measures. The Pearson Chi-square test was applied to determine the statistical significance of association at 5% level of significance. The data was analyzed using SPSS software, version 10.0. Definition of terms used were: Tried/smoked before: one who has only tried smoking and is not a smoker now, or one who has previously smoked but is currently not a smoker; Never tried: one who has never tried smoking in his life; Current smoker: one who smokes currently, regardless of frequency and amount smoked. Mean age of subjects was 16.46 years. Current smokers comprised 35.92% of 451 male students surveyed. Vocational school students had the highest proportion of smokers. Among non-smokers, 187 students had smoked some time in their lives. Mean duration of smoking was 2.49 years. Approximately two-thirds of the smokers started the smoking habit before the age of 15. A total of nearly 21% of the students smoked daily for more than three years (Table 1 ). A significant proportion of the smokers (41.98%) smoked more than 10 cigarettes per day. There was a significant association between the smoking habit of the fathers and that of the students (p < 0.01) (Table 2 ). Reasons most often given for smoking were: following friends, feeling of maturation, enjoyment, following parents, relaxation in free time, and feeling that smoking is the normal behavior of a man (Figure 1 ). Non-smokers most often cited religion, parents' influence, health protection, and financial reasons as factors preventing them from smoking (Figure 2 ). 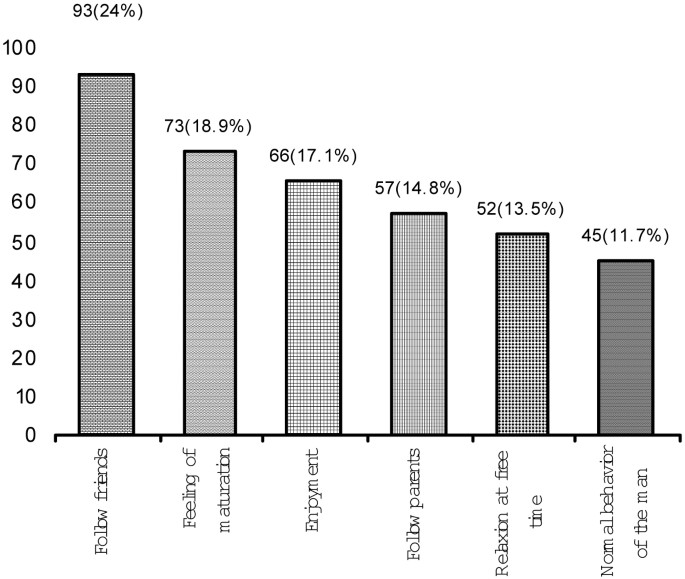 Reasons for smoking, among smokers . 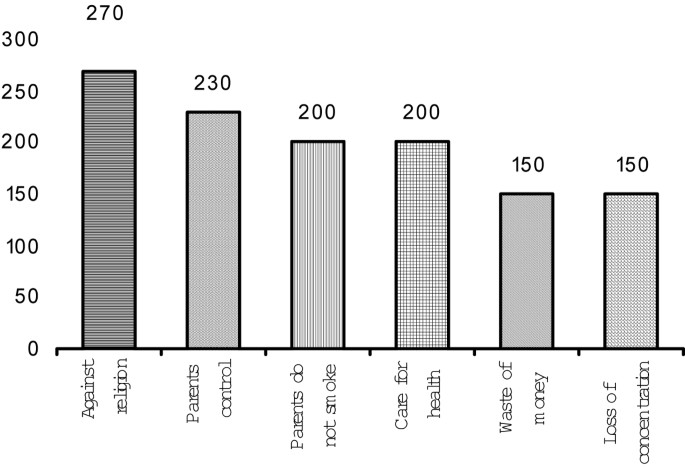 Reasons for not smoking, among non-smokers . The perception of the health hazards of smoking was significantly different between smokers and non-smokers (p < 0.001) (Table 2 ). Smokers had relatively poor academic performance compared to non-smokers (p < 0.001) (Table 2 ). The proportions of smokers in the three schools were significantly different (p < 0.001). The vocational school had the highest number of smokers compared to the other two (Table 2 ). About 60% of smokers had thought of quitting smoking and of these nearly 45% had tried at least once to quit (Table 3 ). Mass media was cited as the best source of information about smoking hazards, followed by medical personnel (Figure 3 ). There was no significant association between source of knowledge and smoking status of the students. 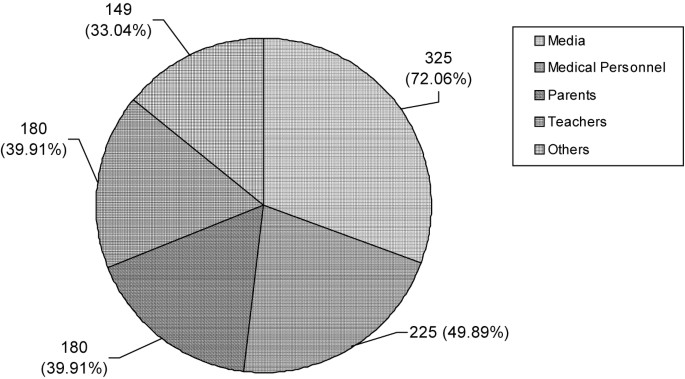 Sources of knowledge about the hazards of smoking . In Kelantan, where the community is relatively conservative, the prevalence of smoking of 35.9% among male adolescents reported by this study was high. The prevalence of male adolescent smoking in Malaysia was reported as 30.7% by the National Health Morbidity survey conducted nationwide in 1996 [ 11 ]. Our study has shown an even higher prevalence than the national level. The authors believe this may be because of the homogeneity of study participants, who were from only the Malay ethnic group. The National Health Morbidity Survey indicated that adolescent smoking was highest in Bumiputras [ 11 ]. The races included under Bumiputra status are Malays and other local tribes. The Non-Bumiputras category includes Chinese and Indians who migrated to Malaysia some decades ago. While the results of our study may not be generalizable to the entire population, this study supports the fact that smoking is a serious problem among the majority ethnic group in the Malaysian population. Among a few locally conducted studies, Thambypillai in 1985 found a prevalence of 17.0% among secondary school boys in urban school in Kuala Lumpur, Malaysia [ 9 ]. In Saudi Arabia, the prevalence of smoking among secondary school boys was only 17% while in China, among middle school students, it was only 2.24% [ 12 , 13 ]. Among the schools where the study was carried out, the highest smoking prevalence was found in vocational school, as expected. Those who entered vocational schools had relatively poorer academic performance than those who went to the other two types of schools. This is no doubt due to the fact that those who fail the qualifying examinations in Form III have to leave school or join vocational or private schools. This study points out that the likelihood of being a smoker increases among academically poorly performing students. Thambypillai in 1985 reported a similar finding of association between high smoking prevalence and poor academic performance [ 10 ]. Our study found that peer influence is the major reason for initiation of smoking; this is similar to findings of other studies [ 14 ]. Peer influence was found to be a strong predictor of smoking initiation in almost all studies that included these measures. Similar findings have been documented by the Surgeon General of the United States [ 2 ]. Two types of peer pressure (i.e., having close friends who smoked, and having close friends who encouraged the student to smoke) were among the strongest risk factors for both regular and occasional smoking. Similar results were found in reports on junior and senior high school students in China [ 15 , 16 ]. Studies from Japan [ 17 ] and Spain [ 18 ] have shown that smoking rates of school students are strongly related to having friends who smoke. This suggests that pupils should be advised to avoid accepting smokers as friends, as the effects are not limited to the odor of tobacco and hazards of passive smoking, but may include pressure to take up this habit. This study found religion was the strongest reason among non-smokers for not smoking. A similar finding has been shown in earlier studies in Saudi Arabia of schoolboys [ 19 ], medical students [ 20 ] and university students [ 21 ]. Smoking has not been declared as "forbidden" from the Islamic religious point of view in Malaysia. However, Malaysia has experienced rapid economic progress in recent years and as the nation has opened to advertising, marketing and imports by international tobacco corporations, smoking rates among teenagers and adolescents have increased [ 22 ]. We recommend that religious education including a religious perspective on the smoking issue should be more emphasized in school curriculum and anti-smoking campaigns, since it is potentially an effective way to educate students especially at the secondary school age. While our study found mass media were the source of information on smoking more than medical personnel, parents, teachers and others, we point out that mass media can not replace face-to-face communication between a student and a doctor, a teacher or parents. Parental smoking has great influence on the children with respect to taking up the smoking habit. There was a significant association between the students' smoking status and their fathers' smoking habits found in this study. The social learning theory of behavior [ 23 ] states that children are more likely to model their own behavior on actions of people they regard as worthy, similar to themselves, and models of their own sex. Two studies [ 24 , 25 ] reported that parental attitude in actively discouraging their children from smoking may be more powerful than parental behavior in shaping adolescent cigarette smoking behavior. Two other studies [ 26 , 27 ] reported that the majority of smokers began their habits in imitation of friends, co-workers or family members. This suggests that in order for campaigns against smoking in adolescents to be most effective, parents must not smoke in the presence of children. More importantly, the children must not be allowed to smoke in their parents' presence. The home environment should complement the school to discipline the students. The role model should be set at home. Academic performance of the students had a highly significant association with the smoking status of the students. Smokers had marked poorer performance than the non-smokers. This finding supports the findings reported by University of Malaya in 1985 in which a higher prevalence of smoking was shown to be associated with poor academic performance [ 28 ]. We call on school authorities to conduct more regular exhibitions and talks, with the help of health personnel, to educate the students about the negative impact of smoking on learning activities. We also recommend that sports and other co-curriculum activities should be encouraged more, in order to provide ways for students to be constructively occupied to prevent them from being attracted to unwanted vice. There was a statistically significant difference in perception towards hazards of smoking between smokers and non-smokers shown by this study. Agreement on the harmfulness of smoking to health was higher among non-smoking students. A similar finding was shown by a study published in 1991 [ 29 ]. Even though smoking may not be regarded as a major discipline problem, the main adverse effects on health are well documented. Smoking is considered the main avoidable cause of death and the most important public health risk. The hazards of tobacco affect not only smokers, but also non-smokers who are exposed to cigarette smoke, "passive smokers." The earlier a person starts smoking, the more difficult it is to quit, the less likely it is that he will quit, [ 30 ] and the greater the risk of lung cancer [ 31 ] or death from coronary heart disease [ 32 ]. The chances of success in quitting decrease as age increases [ 33 ]. To develop and implement effective measures of smoking control, one must understand the reasons and risk factors for smoking initiation. Information about health hazards is usually insufficient for change; studies in Indonesia and other countries in Asia confirmed the observation that knowledge of health risks does not prevent children from smoking [ 34 ]. In addition to demonstrating the hazards of smoking, the benefits of quitting should also be stressed. This study found that more than 50% of regular and occasional smokers expressed their wish to stop smoking. Nearly 45% of them attempted quitting, though a significantly higher proportion was found among occasional smokers. This shows that there was a desire to quit smoking despite the fact that it is difficult to stop the habit once it has become established. While new and innovative approaches to smoking prevention and cessation are being sought, the addictive nature of cigarette smoking and the health advantages of stopping smoking should be given further emphasis in current prevention programs among adolescents. Community and school education programs should include sessions on quitting smoking since there are scientifically proven cessation methods available now. Efforts to prevent experimentation with smoking must also be given higher priority. Promising strategies may include a ban on cigarette advertising and higher tobacco taxes. There is considerable evidence that tobacco advertising and promotion encourage adolescents to smoke [ 35 , 36 ] and that increasing the price of cigarettes discourages young people from starting to smoke. This study focused on smoking behavior on male adolescents. Schoolgirls were not included in the study because in the cultural setting chosen for the study smoking is considered primarily a problem of males, and because of the small sample size of the girls in the schools which were chosen to be included in the study. Also, an unpublished report by the state education department authorities indicated a very small proportion of the smokers among Muslim girls. However, the National Health Morbidity Survey conducted in 1996 reported that the prevalence of female adolescent smoking was as high as 4.8% [ 10 ]. This was an alarming reminder to parents in Malaysia that girls, as well as boys, are at risk to take up smoking. Other studies [ 10 , 26 , 37 ] conducted in Western countries show a higher percentage of smokers among boys and girls of the same age. Given the increasing influence of western culture in Asia and other parts of the world, we would recommend a study exploring smoking behavior among Malaysian female adolescents. The magnitude of the smoking problem in adolescents is large enough to be considered a warning of an impending epidemic. Intervention programs that focus on behavior modification of adolescents should be carried out on a large scale. Multi-centered studies with a homogenous population would be appropriate to measure the effectiveness of intervention strategies. World Health Organization (WHO): Reported by the Director-General, WHO program on tobacco or health E13 77/22 Add 1 Geneva 1995. Preventing Tobacco Use among Young People: A Report of the Surgeon General. 1994, Atlanta, Georgia: Public Health Service. Centers for Disease Control (CDC) and Prevention Google Scholar Reducing the Health consequences of Smoking: 25 Years of Progress. A Report of the Surgeon General. 1989, Washington DC: US Dept of Health and Human Services. DHHS Publication of Centre for Disease Control (CDC), 11: 84-89. Choon NS: Understanding Coronary Artery Disease. Medical Tribune. 1996, 9: 6-7. Horn D: Behavioral aspects of cigarette smoking. Journal of Chronic Diseases. 1963, 16: 383-395. 10.1016/0021-9681(63)90115-2. Article CAS PubMed Google Scholar Fakta Masalah Sosial Remaja: Minda Pelajar. 1995, 79. A study Group of the Public Health Department: The Smoking habits of school children. British Journal of Preventive and Social Medicine. 1959, 13: 1-4. PubMed Central Google Scholar O' Connel DL, Alexander HM, Dobson AJ, Lloyd DM, Hardes GR, Spring thorpe HJ, Leeder SR: Cigarette smoking and drug use in school children. Eleven factors associated with smoking. International Journal of Epidemiology. 1981, 110: 223-231. Salber EJ, Goldman E, Buka M, Welsh B: Smoking habit of high School students in Newton, Massachusetts. New England Journal of Medicine. 1961, 265: 969-974. Thambypillai V: Smoking among urban Malaysia School Children. Social Science and Medicine. 1985, 21: 819-823. 10.1016/0277-9536(85)90130-3. Abdullah S: National Health Morbidity Survey: Health risk behavior among adolescents. Ministry of Health Malaysia. 1996, 133-135. Al-Faris EA: Smoking habits of secondary School boys in Rural Riyadh. Public Health. 1995, 109: 47-55. 10.1016/S0033-3506(95)80075-1. Hu J, Liu R, Zhang H: A Survey of cigarette smoking among middle School Students in China. Public Health. 1990, 104: 345-351. 10.1016/S0033-3506(05)80527-X. Aitken PP: Peer group pressures, parental controls and cigarette smoking among 10–14 year olds. British Journal of Social and Clinical Psychology. 1980, 19: 141-146. Zhu BP, Liu M, Wang SQ: Cigarette smoking among junior high school students in Bejing, China in 1988. International Journal of Epidemiology. 1992, 21: 854-861. 10.1093/ije/21.5.854. Wang SQ, Yu JJ, Zhu BP, Liu M, He GQ: Cigarette smoking and its risk factors among senior high school students in Bejing, China in 1988. Tobacco Control. 1994, 3: 107-114. 10.1136/tc.3.2.107. Article PubMed Central Google Scholar Kawabata T, Maruya N, Nakamura M: Smoking and alcohol drinking behavior among Japanese adolescents: results from 'Japan know your body study'. Nippon-Koshu-Eisei-Zasshi. 1991, 38 (12): 885-899. CAS PubMed Google Scholar Auba J, Villalbi JR: Tobacco and adolescents: influence of personal environment. Medicina Clinica Barcelona. 1993, 100 (3): 506-509. CAS Google Scholar Rowlands DF, Shipster PJ: Cigarette smoking amongst Saudi schoolboys. Saudi Medical Journal. 1987, 8 (6): 613-618. Mostafa A, Aboulfotoh , Mostafa AA, Wole A, Abdullah , Majed SK: Smoking habits of medical students at King Saud University, Riyadh. Annals of Saudi Medicine. 1992, 13 (6): 510-513. Taha A, Bener A, Noah MS, Saeed A, Al-Harthy S: Smoking habits of King Saud university students in Riyadh. Annals of Saudi Medicine. 1991, 11 (2): 141-143. Naing NN, Ahmad Z: Smoking and Discipline problems among rural secondary school students in Kelantan. Malaysian Journal of Medical Sciences. 1997, 4 (1): 54-58. Social Learning and Personality Development. 1963, New York. Holt, Rinehart and Winston Eiser J, Morgan RI, Gammage MP, Gray E: Adolescent smoking: Attitudes, norms and parental influence. British Journal of Social Psychology Part 3. 1963, 193-202. Newman IM, Ward JM: The influence of parental attitude and behavior on early adolescent cigarette smoking. Journal of School Health. 1989, 59 (4): 150-152. Baugh JC, Srinivasan SR, Sklov MC, Berenson GS, Hunter SM: Developmental trends of first cigarette smoking experience of children. The Bogalusa Heart Study. American Journal of Public Health. 1982, 72 (10): 1161-1164. 10.2105/AJPH.72.10.1161. Article PubMed Central CAS PubMed Google Scholar Paine PA, Amaral JA, Pereira MG: Association between parental and student smoking behavior in a Brazilian Medical School. International Journal of Epidemiology. 1985, 14: 330-332. 10.1093/ije/14.2.330. Pathmanathan I: Cigarette smoking among students in the University of Malaya. American Journal of Public Health. 1970, 10: 29-33. Virgili M, Owen N, Sverson HH: Adolescents' smoking behavior and risk perception. Journal of Substance Abuse. 1991, 3 (3): 315-324. Flay BR, Koepke D, Thomson SJ, Santi S: Six-year follow-up o f the first Waterloo school smoking prevention trial. American Journal of Public Health. 1989, 79 (10): 1371-1376. 10.2105/AJPH.79.10.1371. Charlton A: Children's opinion about smoking. Journal of the Royal College of General Practice. 1984, 34: 483-487. Fielding JE: Smoking: Health effects and control. New England Journal of Medicine. 1985, 313 (8): 491-498. Lennox AS: Determinants of outcome in smoking cessation. British Journal of General Practice. 1992, 42: 247-252. PubMed Central CAS PubMed Google Scholar Mackay J: Combating addiction in developing countries. Smokers: Why Do They Start – And Continue?. Edited by: Chapman S. 1995, World Health Forum, 16: 1-27. Pierce JP, Lee L, Gilpin AE: Smoking initiation by adolescent girls, 1944 through 1988. An association with targeted advertising. JAMA. 1994, 271: 608-611. 10.1001/jama.271.8.608. Altman DG, Grimes DA, Chalmers I, Schulz KF: Sustained effects of an educational program to reduce sales of cigarettes to minors. American Journal of Public Health. 1994, 18: 39-42. Rawhone RG, Keeling CA, Jenkins A, Guz A: Cigarette smoking among secondary children in 1975. Journal of Epidemiology and Community Health. 1978, 32: 53-58. 10.1136/jech.32.1.53. Article Google Scholar Download references AcknowledgementsWe would like to express our heartfelt thanks to authorities from the Kelantan state education department, headmasters, teachers, and students from three schools who participated in the study. Author informationAuthors and affiliations. Department of Community Medicine, School of Medical Sciences Universiti Sains Malaysia, 16150, Kubang Kerian, Kelantan, Malaysia Nyi Nyi Naing, Zulkifli Ahmad, Razlan Musa, Farique Rizal Abdul Hamid, Haslan Ghazali & Mohd Hilmi Abu Bakar Department of Community Medicine, School of Medical Sciences, Universiti Sains Malaysia, 16150, Kubang Kerian, Kelantan, Malaysia Nyi Nyi Naing You can also search for this author in PubMed Google Scholar Corresponding authorCorrespondence to Nyi Nyi Naing . Additional informationCompeting interests. The authors declare that they have no competing interests. Rights and permissionsReprints and permissions About this articleCite this article. Naing, N.N., Ahmad, Z., Musa, R. et al. Factors Related to Smoking Habits of Male Adolescents. Tob. Induced Dis. 2 , 133 (2004). https://doi.org/10.1186/1617-9625-2-3-133 Download citation Published : 15 September 2004 DOI : https://doi.org/10.1186/1617-9625-2-3-133 Share this articleAnyone you share the following link with will be able to read this content: Sorry, a shareable link is not currently available for this article. Provided by the Springer Nature SharedIt content-sharing initiative
Tobacco Induced DiseasesISSN: 1617-9625
An official website of the United States government The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site. The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
School policies for preventing smoking among young peopleSchool tobacco policies (STPs) might prove to be a promising strategy to prevent smoking initiation among adolescents, as there is evidence that the school environment can influence young people to smoke. STPs are cheap, relatively easy to implement and have a wide reach, but it is not clear whether this approach is effective in preventing smoking uptake. To assess the effectiveness of policies aiming to prevent smoking initiation among students by regulating smoking in schools. Search methodsWe searched seven electronic bibliographic databases, including the Cochrane Tobacco Addiction Group specialized register, MEDLINE, EMBASE, PsycINFO and ERIC. We also searched the grey literature and ongoing trials resources. The most recent search was performed in May 2014. Selection criteriaWe included cluster‐randomised controlled trials (c‐RCTs) in which primary and secondary schools were randomised to receive different levels of smoking policy or no intervention. Non‐randomised controlled trials, interrupted time series and controlled before‐after studies would also have been eligible. Cross‐sectional studies were not formally included but we describe their findings and use them to generate hypotheses to inform future research. Data collection and analysisWe independently assessed studies for inclusion in the review, and present a narrative synthesis, as the studies are too limited in quality to undertake a formal meta‐analysis. Main resultsWe found only one study which was eligible for inclusion in the review. It was judged to be at high risk of bias. The study compared two 'middle schools' from two different regions in China. The experimental conditions included the introduction of a tobacco policy, environmental changes, and communication activities, while the control condition was no intervention. After a year's follow‐up the study found no differences in smoking prevalence between intervention and control schools. We also described 24 observational studies, the results of which we considered for hypothesis generation. In these, policy exposure was mainly described using face‐to‐face interviews with school staff members, and the outcome evaluation was performed using self‐administered questionnaires. Most studies reported no differences in students' smoking prevalence between schools with formal STPs when compared with schools without policies. In the majority of studies in schools with highly enforced policies, smoking bans extended to outdoor spaces, involving teachers and including sanctions for transgressions, with assistance to quit for smokers plus support by prevention programmes, there was no significant difference in smoking prevalence when compared to schools adopting weaker or no policies. Authors' conclusionsDespite a comprehensive literature search, and rigorous evaluation of studies, we found no evidence to support STPs. The absence of reliable evidence for the effectiveness of STPs is a concern in public health. We need well‐designed randomised controlled trials or quasi‐experimental studies to evaluate the effectiveness of school tobacco policies. Plain language summaryDo school tobacco policies prevent uptake of smoking? Background: We reviewed the evidence that School tobacco policies (STPs) might prevent smoking initiation among adolescents, as there may be some evidence that the school environment can influence young people to smoke. STP is intended to regulate whether and where pupils can smoke, adult smoking in school, and penalties for pupils caught smoking. We were also interested to know whether specific components of STPs might increase their impact. Components such as a smoking ban for students and/or teachers and their extent, levels of enforcement, monitoring strategies, sanctions for students or teachers found smoking, and the offer of tobacco cessation programmes. Study characteristics : Our study search was conducted in May 2014. We identified one c‐RCT from China that we judged to be at high risk of bias. We also focussed on 24 observational studies to generate a hypothesis for future research. Key findings : In the only included c‐RCT with 1807 participants, the intervention did not significantly affect students' smoking behavior. The majority of observational studies reported that schools with highly enforced policies, smoking ban extended to outdoor spaces, involving teachers and including sanctions for transgressions, with assistance to quit for smokers plus support by prevention programmes, did not show a significant difference in smoking prevalence, when compared to schools adopting weaker or no policies. Quality of the evidence : We found no relevant high‐quality experimental studies. A great limitation within observational studies is the heterogeneity of exposure definitions. There is large variability in policy formats, which can include several different characteristics, which in turn makes comparison difficult. Only a few studies are based on policy definition in written documents, while in the majority the information was obtained by interviewing school heads, teachers or administrators. With regard to analysis methods, some studies did not mention any adjustment for potential confounders and in the others there was a large variability in the factors considered for adjustment. Studies differed in statistical methods employed to examine the relationship between policy and smoking behaviour. Conclusions : We cannot draw conclusions about the effectiveness of STP from currently available data. Large, possibly multi‐centric studies, employing experimental or a quasi‐experimental design to assess the effectiveness of STPs are needed. Characteristics that could be studied are: degree of formality, participants to which the policy applies, extension of the ban (indoor areas or external school premises), level of enforcement, sanctions for transgression; assistance with smoking cessation and combination with prevention and education activities. The authors of the review did not receive any external funding or grants to support their research for this review, and have no potential conflicts of interest. Summary of findingsFor the main comparison.
1 Only one study with small number of clusters judged at high risk of bias. Description of the conditionTobacco smoking is an addictive behaviour associated with over five million deaths per year. The World Health Organization projects that the number of deaths per year attributable to tobacco smoking will rise to eight million by 2030. Tobacco use is a major preventable cause of morbidity and mortality, killing an average of one person every six seconds, and is responsible for one in ten adult deaths worldwide ( WHO 2012 ). Though the majority of smoking‐related deaths are in people aged 35 years or older, the onset of tobacco use occurs primarily in early adolescence, and adolescents are a special target for smoking prevention projects. Trends in youth smoking show a decline during the 1970s and 1980s, and an increase in the 1990s in both the USA and Europe ( Warren 2008 ). A younger age of smoking initiation is associated with smoking more cigarettes per day ( Everett 1999 ) and with a lower cumulative probability of quitting ( Chen 1998 ) than in people who start smoking later on in life. Delaying the onset of smoking may affect the likelihood of becoming addicted to nicotine and smoking heavily. Schools have been considered an ideal site to deliver tobacco prevention programmes since they universally involve youths across a wide age range, including the ages when most young people initiate smoking. Generally school programmes show relatively weak effects in reducing adolescent smoking, and these modest results have been explained by the strong social influence effect in favour of smoking inside and outside school premises ( Friend 2011 ). Early studies suggested the role of peer and parental smoking as moderators of school‐based effects ( Tyas 1998 ; Faggiano 2010 ), and perceived smoking by friends has been found to be a stronger predictor of cigarette use than friends' actual use ( Iannotti 1992 ). Some authors have therefore stressed the need to address adolescent smoking at the environmental level ( Griesbach 2002 ; Nakamura 2004 ). Although smoking bans in school settings are common worldwide, because of their low enforcement adolescents are still frequently exposed to teachers and other pupils smoking during the school day. In a study conducted in 48 Danish schools, three in five students reported that they had seen or knew of teachers smoking outdoors on the school premises; and most of them reported that they had seen or knew of teachers smoking inside the school building ( Poulsen 2002 ). In the same study, teachers smoking outdoors on school premises were significantly associated with students' smoking behaviour, while exposure to other pupils smoking outdoors was not. Furthermore, it could be argued that students in a school without anti‐tobacco policies would perceive smoking as being acceptable, increasing their risk of taking up the habit. Description of the interventionAs an intervention, school tobacco policy (STP) is intended to inform whether and where pupils can smoke, to set penalties for pupils caught smoking, and to regulate adult smoking in school ( Evans‐Whipp 2004 ). The primary objectives of this intervention are to prevent or delay tobacco use by youth, and also to reduce the exposure of employees and students to second‐hand smoke. In many cases the introduction of an STP is combined with other smoking prevention programmes. For example, Ariza 2008 describes a multi‐modal intervention, which includes specific lessons for students and strategies to involve adults in smoking cessation programmes. Policies can vary depending on the extent of the ban, teacher and staff training, and the roles and responsibilities of teachers and staff in policy enforcement. Policy can be governed by a central authority at regional or national level rather than locally, and the mandatory nature of a law may moderate its effect on implementation and impact. Other consequences of STPs have also been observed, e.g. schools which do not accommodate student smoking in a specific area can result in adolescents, sometimes in large groups, leaving school property during school hours to smoke elsewhere ( MacBride 2005 ). How the intervention might workFrom the perspective of social learning theory, the interplay between individual and environment is crucial in developing intentions, expectations and ultimately behaviour ( Bandura 1986 ). Cognitive processes such as perceived health risks or benefits of smoking and perceived availability of tobacco could be involved In smoking behaviour. According to Eccles and Roeser’s ecological perspective ( Eccles 1999 ), factors such as peer and adults' smoking habits influence adolescents’ behaviour in combination with other factors. Therefore STPs, implemented as a part of a comprehensive approach, may affect smoking indirectly by influencing beliefs about acceptability (approval or disapproval) of cigarette smoking by adults and by peers ( Lipperman‐Kreda 2009a ). According to identity theory, it has been hypothesised that a strong condemnation of smoking by the school communicates to young people that smoking is an unacceptable part of mainstream identities ( Lloyd 1998 ). A further possibility is that STPs strengthen the connection to school among students and staff, as well as school ethos beyond its regulatory content ( Fletcher 2008 ). An STP can also reduce youth smoking by directly limiting smoking opportunities and access to tobacco ( Alesci 2003 ). The teachers' perceived capacity to act as role models is an important element of the success of this type of intervention. Galaif 1996 found that teachers will comply with a smoking regulation only if they believe that they can directly affect students' smoking behaviour. If students who smoke perceive that it is acceptable for teachers to smoke in school, they are less likely to adhere to school smoking bans. For this reason Trinidad 2005 argues that encouraging teachers not to smoke on school grounds should be considered as a key component of school‐based tobacco prevention programmes; however, conversely smoking bans may encourage teachers to smoke outside school, with the unanticipated result of making teachers who smoke even more visible to students ( Wold 2004 ). Why it is important to do this reviewImplementing STPs was described as a promising strategy to prevent smoking initiation among adolescents ( Bowen 1995 ) However, it is not yet clear whether this approach is effective. It is unclear whether policies contribute to a reduction of youth smoking only when they are included in a comprehensive tobacco control plan at the school level ( Lovato 2010a ), or whether a policy constitutes a suitable and cost‐effective stand‐alone intervention ( Reid 1999 ). A summary of evidence is critical in order to define which STP elements are effective, and which require further research. To assess the effectiveness of policies aiming to prevent smoking initiation among students by regulating smoking in schools. We addressed the following questions:
Criteria for considering studies for this reviewTypes of studies. We include cluster‐randomised controlled trials (c‐RCTs) in which schools or classes were randomised to receive different levels of smoking policy or no intervention. As we expected to find a limited number of RCTs, if any, the following prospective designs were also eligible; non‐randomised controlled trials, interrupted time series and controlled before‐after studies. Cross‐sectional studies were not formally included. In the absence of higher quality evidence, their findings were described and used to generate hypotheses for future studies. Types of participantsStudents in primary and secondary schools (10 to 18 years old). Types of interventionsAll written policies that regulate tobacco use inside and/or outside the school property were eligible. We would have classified interventions as partial bans, inside bans and comprehensive policies. We would have included studies of policies aiming to ban drug or alcohol use in addition to smoking if tobacco use outcomes were reported. We would have considered interventions in which an STP was a component of a smoking prevention program only if it was possible to isolate its effect. Studies that compared stronger and weaker policies were eligible. We would have considered whether the implementation of a policy had an impact on its effect. Types of outcome measuresPrimary outcomes. Smoking prevalence among students, measured by individual self‐report. Biochemically validated smoking data, where provided, were used in preference to self‐report. Young people were classified as smokers or non‐smokers in different ways (daily, weekly, monthly, ever, non‐smoker, smokeless tobacco user, smoker). Where multiple definitions were provided, we used the strictest measure given. In studies with multiple follow‐up periods, we would have used data from the longest follow‐up period reported. Secondary outcomes1. Actual tobacco use by teachers and school staff. 2. Tobacco use of teachers, school staff, and students as perceived by other students. 3. Compliance with the policy by students, teachers and school staff. 4. Exposure to environmental tobacco smoke.  Search methods for identification of studiesWe conducted the most recent search in May 2014. We searched the following databases: 1. Cochrane Tobacco Addiction Group's Specialised Register 2. Cochrane Central Register of Controlled Trials (CENTRAL) 3. MEDLINE 4. EMBASE 5. PsycINFO 6. ERIC (Educational Resources Information Center) 7. Sociological abstracts (CSA) 8. 'Grey' literature (conference proceedings and unpublished reports) via Google Scholar and dissertation abstracts. 9. Unpublished literature, by searching trial registers (www.clinicaltrials.gov, www.controlled‐trials.com, www.clinicaltrialsregister.eu) and contacting researchers and agencies whom are known to have conducted or sponsored relevant research to identify further studies not found and unpublished reports. The Tobacco Addiction Group Specialized Register contains reports of controlled trials of interventions for smoking cessation or prevention, evaluations of tobacco control policies, identified from regularly updated highly sensitive searches of CENTRAL, MEDLINE, EMBASE, PsycINFO, and the Science Citation Index. The search strategy for the register used the following topic related terms; (polic* or ban* or restriction* or rule* or environment* or health promoting or smoke‐free) AND (school*) in title, abstract or keyword fields. The search strategies for MEDLINE, EMBASE and PsycINFO combined these topic terms with the smoking and tobacco terms and the study design terms used for the Register searches. The full MEDLINE search strategy can be found in Appendix 1 . Searches of ERIC, Sociological Abstracts and other sources combined topic related and smoking related terms. Searching other resourcesWe checked cited studies in all studies identified. We did not apply language restrictions. In the case of languages other than English, French, German, Italian, Spanish, Portuguese, Greek, Russian or Swedish, we would have looked for translation facilities within the Cochrane Collaboration. Selection of studiesAll search results were imported into an electronic register. Titles and abstracts were classified according to their relevance to the review. Once bibliographic searches was completed, all retrieved records were assembled in a database and processed in order to de‐duplicate them (i.e., remove duplicate records). Two reviewers (AC, FF) screened all identified studies in the electronic databases. Articles were rejected if the title or abstract was not pertinent to the topic of the review. Any disagreements was resolved between the two reviewers by referring to the full‐text, and by consulting with a third party when necessary (MRG). The same reviewers conducted further screening of the full text of the studies that passed the initial screening stage. Data extraction and managementTwo reviewers (AC, FF) independently extracted data from the selected study using a tailored standardised data extraction form including the following elements:
Any discrepancies were resolved through discussion or, if required, through consultation with a third person (MRG). Assessment of risk of bias in included studiesTwo review authors assessed independently risk of bias for each study using the criteria outlined in the Cochrane Handbook for Systematic Reviews of Interventions ( Higgins 2011 ): • adequate sequence generation; • adequate allocation concealment; • blinding of personnel/outcome assessors; • addressing incomplete outcome data; • free of selective outcome reporting; • free of other bias. For each of these domains, risk of bias was judged High, Low, or Unclear Any disagreement was resolved by discussion or by involving a third assessor. Measures of treatment effectFor dichotomous data, we used the risk ratio (RR) to summarize individual trial outcomes ((number of events in intervention condition/ intervention denominator)/ (number of events in control condition/control denominator)) with 95% confidence intervals. For our primary outcome, the RR was calculated using the student population of the school as the denominator ((number of student smokers in intervention condition/student population in intervention condition)/(number of student smokers in control condition/student population in control condition)). Where the event measured was students classified as smokers, a risk ratio less than one indicated that fewer students were smokers in the intervention group than in the control group. For continuous data, we used the mean difference if outcomes were measured in the same way between trials. We used the standardised mean difference to combine trials that measured the same outcome, but use different methods. Unit of analysis issuesThough in cluster randomised trials we expected the school (or classes) to be the unit of randomisation, we used the individual as the unit of analysis. We reported adjustments for design effect when provided and dealt with any unit of analysis issues using the guidance in the Cochrane Handbook for Systematic Reviews of Interventions ( Higgins 2011 ). Dealing with missing dataIf the proportion of missing data suggested a risk of bias, the study would have been classified accordingly and included in a sensitivity analysis. Participants who has been missing follow‐up data for our primary outcome would have been counted as smokers in an intention‐to‐treat analysis. Assessment of heterogeneityThe statistical heterogeneity was to be examined using the I 2 statistic. However, this was not necessary as we included only one study. Assessment of reporting biasesHad we found sufficient studies, we would have tested publication bias using a funnel plot. The relevance of outcomes had been checked to determine if there was any bias in outcome reporting. Data synthesisIf we had found sufficient studies we would have carried out summary analyses using RevMan 5.1. We would have used the Mantel‐Haenszel fixed‐effect model for meta‐analyses, combining data where trials examined the same intervention and populations and methods were judged sufficiently similar. Where we had suspected clinical or methodological heterogeneity between studies sufficient to suggest that treatment effects may differ between trials, we would have used a random‐effects meta analyses. Subgroup analysis and investigation of heterogeneityIf relevant studies had been available, we would have conducted subgroup analyses for the following policy characteristics: • ban extended only to school staff versus extended both to staff and students; • only indoor area affected by the ban versus ban extended to outdoor area; • policies enforced by punishment versus policies not enforced by punishment; • policies as stand‐alone interventions versus policies accompanied by educational programmes. In the presence of substantial heterogeneity, we would have explored the reasons for this, undertaking sensitivity analyses (if there have been sufficient studies to warrant this approach). Description of studiesResults of the search. Figure 1 shows the study selection process (up to May 2014). Two review authors (AC, FF) independently assessed all the titles and abstracts identified as a result of the comprehensive updated search. Initially 2182 citations were identified in the electronic databases, of which 1702 remained after de‐duplication. No ongoing studies were found in trial registers. We excluded 1553 studies after screening the titles and then 90 after reading the abstracts. At the end of selection process we included one study in this review, which aimed to study the effect of the introduction of smoking policies at school.  Study flow diagram Included studiesThe included study ( Chen 2014 ) was conducted in 2008 in two Chinese regions and involved two schools in the intervention group and two in the control group. Of a total of 1807 participants aged between 13 and 15 years old, 941 students attended intervention schools and 866 attended control schools. The students were then surveyed a year later about their smoking habits. To assess the frequency of smoking, participants were asked whether they smoked daily, weekly, or were smoking currently. Ever‐smoking was defined as having ever used cigarettes, even one or two times. Characteristics of the intervention were: smoking banned inside the school; peer educators trained to encourage smokers to quit; and brochures about health hazards of smoking distributed among students. The study measured changes in students' smoking behaviour, knowledge and attitudes. The Characteristics of included studies table provides further details on participants, interventions, and outcomes of the study. Excluded studiesAmong the 58 studies that were excluded, 51 were observational and therefore not eligible. Seven studies were randomised controlled trials (RCTs) ( Andersen 2012 , Elder 1996 , De Vries 2006 , Gorini 2014 , Hamilton 2005 , Schofield 2003 , Wen 2010 ), evaluating multi‐modal programmes, but it was not possible to disentangle the effect of STP from those of others interventions, and so they were excluded. Of the 51 observational studies, 27 reported a predictor not suitable for this review (STP not sufficiently specified) or no outcome suitable for the review. The Characteristics of excluded studies table provides details of the respective reasons for excluding each study. The remaining 24 studies reported an effect on students' smoking behaviour and information about the policies' characteristics was collected through interviews with school staff. Even if excluded from the review, they were considered useful for hypothesis generation. All but one were cross sectional studies, while one ( Rosendhal 2002 ) was a cohort study. Twenty‐two studies involved middle or secondary schools, and two were conducted in primary schools ( Rosendhal 2002 ; Huang 2010 ). Information about the study, characteristics of the policy and main results are summarised in Table 2 .
All the studies are cross‐sectional with the exception of Rosendhal 2002 that is a cohort study. Risk of bias in included studiesThe only study included ( Chen 2014 ), had a small sample size of only 4 schools, a high risk of intraclass correlation, a likely absence of blinding, and lack of information to assess the presence of selective reporting; we judged the risk of bias of this study to be very high. This assessment is summarised in Figure 2 .  Risk of bias summary: review authors' judgements about each risk of bias item for each included study. Effects of interventionsSee: Table 1 In Chen 2014 a school tobacco policy (STP) was not significantly associated with all smoking outcomes studied. There weren't substantial differences in the prevalence of current smokers between intervention and control schools in either of the two regions: risk ratio (RR) 0.98 (95% CI 0.71 to 1.4) and RR 1.35 (95% CI 0.57 to 3.2). The study didn't consider other outcomes of interest for this review. Studies considered for hypothesis generationUsing data from 24 observational studies, we were interested if specific characteristics of STPs were associated with students smoking behaviour. The characteristics analysed were the following:
The mere adoption of an STP did not seem to affect smoking behaviour. Nine studies measured the effects of a formally‐adopted STP on students' smoking. These studies present mixed results, as three studies showed lower prevalence of smoking in schools with STPs, when compared with schools without a formal policy ( Lovato 2010b ; Moore 2001 ; Sinha 2004b ), while six studies reported no differences ( Galán 2012 ; Hamilton 2003 ; Huang 2010 ; Murnaghan 2007 ; Murnaghan 2008 ; Rosendhal 2002 ). We also analysed the effects of five aspects of policy: extent of a smoking ban, inclusion of teachers' smoking, sanctions for transgression, assistance for smoking cessation, and a ban combined with prevention and education activities. Only a few studies reported results to support the effects of these features. With respect to the extent of bans, one study detected a difference in students' smoking prevalence, when comparing schools which prohibited students’ smoking on school premises or outdoors, with those which permitted smoking ( Piontek 2008b ). Three studies found no differences ( Barnett 2007 ; Huang 2010 ; Pentz 1989 ); however, of these Pentz 1989 found a difference only in the number of cigarettes smoked. One policy forbidding teachers to smoke was associated with a decrease in students' daily smoking ( Kumar 2005 ). Prohibition of indoor smoking for teachers was not significantly associated with student smoking, while prohibiting teachers from smoking outdoors was associated only with decreased daily smoking in girls aged 13 years, but not among boys and girls aged 16 years ( Barnett 2007 ). In Boris 2009 , Clarke 1994 , Piontek 2008b , and Wiium 2011a , comprehensive policies prohibiting teachers from smoking, when compared with those allowing them to smoke in restricted areas, were not related to student smoking. Nine studies considered the relationship between sanctions for students found smoking and smoking prevalence. Sanctions cited in the STP were not related to smoking prevalence in the majority of the studies ( Darling 2006 ; Pentz 1989 ; Piontek 2008b ; Wiium 2011a ). Harsh and remedial penalties ( Evans‐Whipp 2010 ), the severity of sanctions ( Kumar 2005 ; Paek 2013 ), and sanctions put in place at school and informing parents ( Wiium 2011b ) were not associated with adolescent smoking. In one study ( Hamilton 2003 ) counselling and education for students caught smoking appeared to be more effective against student smoking than a disciplinary approach alone. Seven studies considered the effect of assistance with smoking cessation for students. Out of these, only Sabiston 2009 showed a link to a lower probability of smoking. Of the others, five studies did not show a link ( Darling 2006 ; Evans‐Whipp 2010 ; Lovato 2007 ; Pentz 1989 ; Piontek 2008b ); in fact Pentz 1989 reported a higher number of cigarettes smoked in schools where cessation support was available. Moreover, Lovato 2010a showed that in schools that mandated cessation programmes students had a higher probability of smoking. Six studies compared the effect of 'STP only' to 'STP with prevention and education components', but did not find an association with reduction of smoking prevalence ( Darling 2006 ; Lovato 2007 ; Murnaghan 2007 ; Murnaghan 2008 ; Pentz 1989 ; Sabiston 2009 ). Pentz 1989 reported lower numbers of cigarettes smoked and lower smoking prevalence (although not statistically significant) in schools with smoking ban policies and smoking prevention programmes. Eleven of the considered studies focused particularly on the role of policy enforcement. Four studies showed that policy enforcement was linked to lower rates of smoking ( Adams 2009 ; Kumar 2005 ; Moore 2001 ; Sabiston 2009 ). In one study, the data were in favour of schools adopting policy enforcement, but the effect was no longer statistically significant after adjustment for state, gender, age and family socioeconomic status ( Evans‐Whipp 2010 ). The presence of an enforcement officer, but not the strength of the enforcement, was associated with a lower probability of smoking in one study ( Lovato 2010a ). Smoking prevalence was not related to policy enforcement in two studies ( Lovato 2007 ; Wiium 2011b ). One study found no difference in smoking prevalence between schools with a high versus a low degree of monitoring of students’ compliance with the policy ( Piontek 2008b ). In contrast, Lovato 2010b found that students were more likely to smoke if they attended a school with stronger enforcement of the tobacco policy. Policy enforcement for teachers was not associated with a difference in daily and weekly smoking among students in one study ( Moore 2001 ). Table 2 shows further details on characteristics, outcomes and results of the considered studies for hypothesis generation, while Table 3 summarizes the effect of policies' characteristics on students' smoking behaviour as reported in the studies.
OR: odds ratio RR: risk ratio Summary of main resultsThe results of this review are limited by the number of studies identified and the low methodological quality of the only one we included, Chen 2014 , which showed no significant differences for students' smoking behaviours between schools with and without a STP. Furthermore, the study was judged as having high risk of bias. For this reason at present there is insufficient evidence that STPs are effective for the reduction of smoking initiation among young people. Through a systematic search of observational studies, we also identified some studies exploring different aspects of STP. Specific characteristics like enforcement, extended outdoor bans, strict surveillance measures, assistance to quit smoking, formal adoption of a STP and inclusion of prevention or education activities were not found to be associated with a decreased likelihood of smoking. These results questioned the effectiveness of STPs, but, given the very low quality of the evidence, in the absence of large and rigorous intervention studies, they should be considered in order to orient future research on this topic. The review didn't include studies that addressed whether STPs are able to reduce the start of smoking in adolescents or reduce the number of cigarettes among smokers. Quality of the evidenceIt is important to consider that the main conclusion of this review is based only on one randomised controlled trial (RCT) at high risk of bias. This is because the included study did not describe the randomisation method for the schools and did not provide information on allocation concealment, which may introduce significant selection bias. On the other hand the number of dropouts and participants lost to follow‐up were very low. Given the characteristics of the assessed intervention, it is important to note that it was not feasible to blind the participants or the school personnel. The investigators measuring the outcomes could have been blinded, but this was not reported in the included study. Insufficient details were provided on variables used In the statistical analysis for the adjustment for possible confounders. We have also analysed some observational studies, which in turn have important limitations, apart from their study design. One important issue is the heterogeneity of exposure definition. There is large variability in policy formats, and these can include several different characteristics, which make comparisons difficult. Only a few studies are based on policy definition in written documents. Policy information obtained by interviewing school principals, school administrators or teachers might overstate the extent of the STP, and frequently it is not possible to differentiate the contribution of the STP from that of other school interventions. Descriptive terms, like 'enforcement' or 'comprehensiveness', were used in different and incompatible ways, with specific policy characteristics being differently defined. This was true of smoking prevention programmes, availability of cessation support, and the sanctions for violations. The outcome variables were heterogeneous, and the age range between studies was variable. Since age is a major determinant of the prevalence of tobacco use, with a doubling of the initiation rates between early and middle adolescence ( DiFranza 2007 ), discrepancies between studies should always be interpreted with respect to age distribution. With regard to analysis methods, some studies did not mention any adjustment for potential confounders ( Clarke 1994 ; Darling 2006 ; Sinha 2004b ; Wiium 2011b ) and in general there is large variability in the factors considered for adjustment. Agreements and disagreements with other studies or reviewsFive RCTs excluded from this review ( Elder 1996 ; De Vries 2006 ; Hamilton 2005 ; Schofield 2003 ; Wen 2010 ), as it was not possible to differentiate the effect of smoking policy from other interventions, were included in another Cochrane review ( Thomas 2013 ). A recent Cochrane review ( Langford 2014 ) aimed to assess the impact of the Health Promoting School framework on several health behaviours; four ( De Vries 2006 ; Hamilton 2005 ; Schofield 2003 ; Wen 2010 ) of 14 studies included for evaluating the effect on smoking behaviour were also considered in this review, but excluded for the reason mentioned above. The conclusions of the present work largely agree with those produced in a previous systematic review ( Galanti 2014 ). Other reviews on STP have previously been published. A review conducted with the scope of identifying which school characteristics are responsible for the variation in smoking prevalence found weak associations between some aspects of STPs and smoking ( Aveyard 2004 ). A narrative review on the impact of school drug policies on youth substance use concluded that more comprehensive and strictly enforced policies are associated with less smoking, but may also displace the behaviour from school grounds to off‐school premises ( Evans‐Whipp 2004 ). A non‐systematic review of school contextual effects on students' behavioural outcomes showed how in schools without STPs, smoking was more prevalent among pupils ( Sellström 2006 ), but no detailed description of the characteristics of the policies was provided. Implications for practiceDespite a comprehensive search of the literature evaluating the effectiveness of school policies for preventing smoking among young people, we did not find any evidence of an effect. This is mainly explained by the absence of rigorous studies. Whlie this finding suggests that STP is an ineffective stand‐alone intervention, we believe that the theoretical basis of this intervention ( Wilson 2012 ) should be tested under the control of well designed studies. Implications for researchLarge, possibly multi‐centric studies, employing an experimental or a quasi‐experimental design, are needed to assess the effectiveness of this intervention. Future research in this area must be rigorously designed and evaluated. Design issues of particular importance include the following:
Several STP components can play an essential role in contributing to policy effectiveness; the most important ones suggested by this review are:
AcknowledgementsThe authors would like to thank the editorial staff of the Cochrane Tobacco Addiction Review Group for running the search strategy and for their advice and support during the review process. Appendix 1. MEDLINE search strategy1 RANDOMIZED‐CONTROLLED‐TRIAL.pt. 2 CONTROLLED‐CLINICAL‐TRIAL.pt. 3 CLINICAL‐TRIAL.pt. 4 Meta analysis.pt. 5 exp Clinical Trial/ 6 Random‐Allocation/ 7 randomized‐controlled trials/ 8 double‐blind‐method/ 9 single‐blind‐method/ 10 placebos/ 11 Research‐Design/ 12 ((clin$ adj5 trial$) or placebo$ or random$).ti,ab. 13 ((singl$ or doubl$ or trebl$ or tripl$) adj5 (blind$ or mask$)).ti,ab. 14 (volunteer$ or prospectiv$).ti,ab. 15 exp Follow‐Up‐Studies/ 16 exp Retrospective‐Studies/ 17 exp Prospective‐Studies/ 18 exp Evaluation‐Studies/ or Program‐Evaluation.mp. 19 exp Cross‐Sectional‐Studies/ 20 exp Behavior‐therapy/ 21 exp Health‐Promotion/ 22 exp Community‐Health‐Services/ 23 exp Health‐Education/ 24 exp Health‐Behavior/ 25 1 or 2 or 3 or 4 or 5 or 6 or 7 or 8 or 9 or 10 or 11 or 12 or 13 or 14 or 15 or 16 or 17 or 18 or 19 or 20 or 21 or 22 or 23 or 24 26 smoking cessation.mp. or exp Smoking Cessation/ 27 "Tobacco‐Use‐Cessation"/ 28 "Tobacco‐Use‐Disorder"/ 29 Tobacco‐Smokeless/ 30 exp Tobacco‐Smoke‐Pollution/ 31 exp Tobacco‐/ 32 exp Nicotine‐/ (19782) 33 ((quit$ or stop$ or ceas$ or giv$) adj5 smoking).ti,ab. 34 exp Smoking/pc, th [Prevention & Control, Therapy] 35 26 or 27 or 28 or 29 or 30 or 31 or 32 or 33 or 34 [A category smoking terms] 36 exp Smoking/ not 35 [B category smoking terms] 37 1 or 2 or 3 [Likely CT design terms; RCTs, CCTs, Clinical trials] 38 35 and 25 [A category smoking+all design terms] 39 35 and 37 [A category smoking terms+likely CT design terms] 40 (animals not humans).sh. [used with 'not' to exclude animal studies for each subset] 41 ((26 or 27 or 28 or 29) and REVIEW.pt.) not 38 [Set 4: Core smoking related reviews only] 42 36 and 25 [B category smoking+all design terms] 43 (42 and 37) not 40 [Set 3: B smoking terms, likely CT design terms, human only] 44 38 not 39 not 40 [Set 2: A smoking terms, not core CT terms, human only] 45 (35 and 37) not 40 [Set 1: A smoking terms, likely CT design terms, human only] 46 (36 and 25) not 40 not 43 [Set 4: B smoking terms, not core CT terms] 47 (polic* or ban* or restriction* or rule* or environment*).mp. 48 school*.mp. 49 47 and 48 [Topic related terms] 50 45 and 49 [Topic + A smoking terms & core CT terms SET 1 ] 51 44 and 49 [Topic + A smoking terms & wide design terms SET 2 ] 52 43 and 49 [Topic + B smoking terms & core CT terms SET 3 ] 53 46 and 49 [Topic + B smoking terms & wide design terms SET 4 ] Lines 1 to 24 identify controlled trials and other types of programme evaluations, as used to identify reports of studies for the Tobacco Addiction Group Specialised Register. Lines 26 to 34 identify reports related to smoking and tobacco control. Lines 47 and 48 identify reports relevant to the topic of this review. Sets 1 to 4 will be screened for the review, Sets 1 and 2 are expected to be the most likely to contain relevant reports, and Set 4 to be unlikely to identify any. Edited (no change to conclusions) Characteristics of studiesCharacteristics of included studies [ordered by study id].
Characteristics of excluded studies [ordered by study ID]
Differences between protocol and reviewBackground section has been summarised from the original protocol. List of eligible study designs now uses EPOC recommended terminology. Contributions of authorsAC was involved in coordinating the review, developing the protocol, extracting data, conducting the analysis and co‐wrote and edited the review. MRG was involved in developing the protocol and co‐wrote the review. LG, DB and SB were involved in conducting the analysis and co‐wrote the review. FF was involved in coordinating the review, developing the protocol, extracting data and co‐wrote and edited the review. Sources of supportInternal sources.
External sourcesParticipant organizations in ALICE RAP can be seen at http://www.alicerap.eu/about‐alice‐rap/partners.html. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Declarations of interestAC, MRG, LG, DB, SB and FF have no potential conflict of interest. References to studies included in this reviewChen 2014 {published data only}.
References to studies excluded from this reviewAdams 2009 {published data only}.
Aldinger 2008 {published data only}
Andersen 2012 {published data only}
Ariza 2008 {published data only}
Baillie 2008 {published data only}
Barnett 2007 {published data only}
Boris 2009 {published data only}
Clarke 1994 {published data only}
Darling 2003 {published data only}
Darling 2006 {published data only}
De Vries 2003 {published data only}
De Vries 2006 {published data only}
Elder 1996 {published data only}
Evans‐Whipp 2007 {published data only}
Evans‐Whipp 2010 {published data only}
Galán 2012 {published data only}
Garcìa‐Vàzquez 2009 {published data only}
Gorini 2014 {published data only}
Griesbach 2002 {published data only}
Hamilton 2003 {published data only}
Hamilton 2005 {published data only}
Huang 2010 {published data only}
Johnson 2009 {published data only}
Kumar 2005 {published data only}
Labiris 2005 {published data only}
Lipperman‐Kreda 2009a {published data only}
Lipperman‐Kreda 2009b {published data only}
Lovato 2007 {published data only}
Lovato 2010a {published data only}
Lovato 2010b {published data only}
Maes 2003 {published data only}
Moon 1999 {published data only}
Moore 2001 {published data only}
Murnaghan 2007 {published data only}
Murnaghan 2008 {published data only}
Murnaghan 2009 {published data only}
Novak 2001 {published data only}
O'Brien 2010 {published data only}
Paek 2013 {published data only}
Pentz 1989 {published data only}
Pinilla 2002 {published data only}
Piontek 2008a {published data only}
Piontek 2008b {published data only}
Poulin 2007 {published data only}
Reitsma 2004 {published data only}
Rosendhal 2002 {published data only}
Roski 1997 {published data only}
Sabiston 2009 {published data only}
Schofield 2003 {published data only}
Sinha 2004a {published data only}
Sinha 2004b {published data only}
Trinidad 2005 {published data only}
Wakefield 2000 {published data only}
Watts 2010 {published data only}
Wen 2010 {published data only}
Wiium 2011a {published data only}
Wiium 2011b {published data only}
Wold 2004 {published data only}
Østhus 2007 {published data only}
Øverland 2010 {published data only}
Additional referencesAlesci 2003.
Aveyard 2004
Bandura 1986
DiFranza 2007
Eccles 1999
Evans‐Whipp 2004
Everett 1999
Faggiano 2010
Fletcher 2008
Friend 2011
Galaif 1996
Galanti 2014
Higgins 2011
Iannotti 1992
Langford 2014
MacBride 2005
Nakamura 2004
Poulsen 2002
Sellström 2006
Thomas 2013
Warren 2008
Wilson 2012
References to other published versions of this review
Advertisement Supported by Bloomberg’s $1 Billion Gift for Free Medical School Applies but Not to AllA donation from Bloomberg Philanthropies will provide free tuition for Johns Hopkins medical students, if their families make less than $300,000 a year.  By Anemona Hartocollis How rich is too rich to receive free tuition at medical school? That is the question raised by the $1 billion gift from Bloomberg Philanthropies to Johns Hopkins University to cover tuition for most of its medical students, announced on Monday. The gift put the charity set up by Michael Bloomberg, a former mayor of New York City, in the same league as the $1 billion donation from Ruth Gottesman , a longtime professor at Albert Einstein College of Medicine in the Bronx and the widow of a Wall Street tycoon. Her gift to Einstein in February promised that no medical student there would ever again have to pay tuition. And New York University’s medical school began covering its students’ tuition in 2018, helped by a $100 million contribution from Kenneth G. Langone , a co-founder of Home Depot, and his wife, Elaine. But there is one key difference among the programs: Mr. Bloomberg’s generosity is means-tested, given only to students whose family income is under $300,000 a year. The programs at Einstein and N.Y.U. cover all medical students, regardless of income, need or merit. Before the Bloomberg gift, tuition at Johns Hopkins came to roughly $65,000 a year for four years, a hefty sum even for a family earning $300,000 a year. The university estimates the overall cost of attending, including living expenses and fees, at more than $102,000 in the first year. What makes $300,000 the right cutoff? And should medical school students be compelled to rely on their parents, however wealthy, for tuition? Aides to Mr. Bloomberg say that the cutoff was carefully calibrated to weigh the total size of the gift — $1 billion — and its maximum impact. We are having trouble retrieving the article content. Please enable JavaScript in your browser settings. Thank you for your patience while we verify access. If you are in Reader mode please exit and log into your Times account, or subscribe for all of The Times. Thank you for your patience while we verify access. Already a subscriber? Log in . Want all of The Times? Subscribe .  | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
IMAGES
VIDEO
COMMENTS
500 Words Essay On Smoking. One of the most common problems we are facing in today's world which is killing people is smoking. A lot of people pick up this habit because of stress, personal issues and more. In fact, some even begin showing it off. When someone smokes a cigarette, they not only hurt themselves but everyone around them.
Understanding smoking's negative effects in its entirety is essential if we want to prevent moral individuals from losing their lives to smoking. 10 Pointer Essay on Smoking. These 10 points provide a brief summary of the whole essay. Students, especially of primary classes can take help from these points to write their essays.
Students are often asked to write an essay on Teenage Smoking in their schools and colleges. And if you're also looking for the same, we have created 100-word, 250-word, and 500-word essays on the topic. ... Smoking among teenagers has become a pressing concern, posing significant risks to their health and overall well-being. ...
The socio-demographic characteristics and cigarette smoking behavior of the students were measured by using a standardized pre-tested self-administrated validated questionnaire in English. The overall prevalence of cigarette smoking among students was found to be 49.4%. The mean age of starting cigarette smoking was 19.2 2.73 years.
Reasons why one may begin smoking, are among the most prominent smoking essay topics. It is not easy to begin to enjoy the habit, as the act of smoke inhalation can be difficult to control due to a lack of experience and unfamiliarity with the concept. ... Consequently, the inequality and discrimination against LGBTQ + students in high school ...
Rates of overall tobacco use remain high, however. In 2015, 25.3% of high school students and 7.4% of middle school students used a tobacco product. 7. Since 1990, teenagers and young adults have had the highest rates of maternal smoking during pregnancy. In 2014, 10.2% of female teens aged 15 to 19 and 13% of women aged 20 to 24 smoked during ...
This finding is in agreement with a study conducted in 1960s that found smokers among adolescents have lower grade compared with a nonsmoker.20 Another study also showed a negative correlation between smoking and academic performance among school students.21 In addition, our findings are supported by several studies showing that increased ...
Smoking alone causes 90% of lung cancer, 80%. of chronic bronchitis, and 25% of other lung-related. diseases. None of the organs in the body are safe from. the harmful effects of tobacco. Smoking ...
This is an essay that is about causes and effects of smoking among students. It is composed of four paragraphs. The main ones in the body are about causes of smoking among students and its bad consequences. This essay is a kind of warning for students to stop smoking. This is an essay that is about causes and effects of smoking among students.
Free essays on Smoking for students. Get plenty of ready-made samples on Smoking or create your own. ️ . Essay Editor; ... Among the most common addictions are alcohol, tobacco, and illicit substance use. The number of deaths due to this problem is 11.8% of the whole, ...
Here is an example of the thesis for this type of smoking among teenagers essay: Caused by peer pressure, smoking negatively affects teenagers' health and appearance. Effectively develop your points. ... For example, if you are writing about smoking students, introduce the shocking statistics at the beginning of your paper and convince them ...
Tobacco use is a global epidemic among young people. As with adults, it poses a serious health threat to youth and young adults in the United States and has significant implications for this nation's public and economic health in the future (Perry et al. 1994; Kessler 1995). The impact of cigarette smoking and other tobacco use on chronic disease, which accounts for 75% of American spending ...
Among all students, perceiving no harm or little harm from intermittent tobacco product use (use on some days but not every day) was 28.2% for e-cigarettes, 16.4% for hookahs, 11.5% for smokeless ...
Abstract. Cigarette smoking and drinking commonly co-occur among college students, a population that is at high risk for developing alcohol and nicotine use disorders. Several studies have been conducted that have examined predictors of drinking or smoking to gain a better understanding of the antecedents of engaging in these behaviors.
Background There is an increase in the use of cigarettes and e-cigarettes worldwide, and the similar trends may be observed in young adults. Since 2014, e-cigarettes have become the most commonly used nicotine products among young adults (Sun et al., JAMA Netw Open 4:e2118788, 2021). With the increase in e-cigarette use and the decrease in use of cigarettes and other tobacco products, however ...
Conclusion: The prevalence of smoking among university students was high compared to previous findings and the trend was even higher in female students. The majority of the smokers were reluctant ...
A cause effect essay The causes and effects of smoking among students Smoking is one of the most dangerous widespread phenomena that threatens lives of a huge number of people worldwide. It starts as a way of having fun, but ends as an addiction that is therefore so difficult to give up. Today, we often hear of "smoking among students".
SMOKING AMONG HIGH SCHOOL STUDENTS tude scale was used also in the reques-tioning of all the students. 7. A special study was made of the effect of a film on smoking, sponsored byanother organization, shownin assem-bly to the students of a school which was among those studied, but not in-cludedin the six experimental groupings. 8.
The average number of cigarettes smoked per day for female is 15 compared to 17 cigarettes for male students. Almost half of the respondents, 56.1% of current smokers trying to quit smoking, while 43.9% had no desire to stop smoking. The average period of abstinence for former smokers was 4.1 ± 2.3 years.
In the first three lessons, students learn different aspects of human subjects research, discuss variation in smoking behavior, and study the biology of nicotine addiction. In lesson 4, students learn the case control study design and epidemiological analysis, including criteria used to distinguish causality from associations . Lesson 5 focuses ...
M Males, younger adolescents, Hispanics, and non-Hispanic blacks were more likely than their peers to view light and intermittent smoking patterns as less harmful, while those who were already light or intermittent smokers, those who used other tobacco products, and those who had a family member who used tobacco were also less likely to view theirsmoking patterns as harmful.
Smoking causes cancer. As a result, the addict students would suffer from health problems that end in death. Another effect is that after certain years, the addict would develop respiratory problems and will face a lot of problems in running without losing breath. So, asthma, bronchitis, and emphysema are always a lingering threat.
A cross-sectional study was conducted to identify the factors related to smoking habits of adolescents among secondary school boys in Kelantan state, Malaysia. A total of 451 upper secondary male students from day, boarding and vocational schools were investigated using a structured questionnaire. Cluster sampling was applied to achieve the required sample size. The significant findings ...
Smoking prevalence among students, measured by individual self‐report. Biochemically validated smoking data, where provided, were used in preference to self‐report. ... Students participated in smoking cessation‐related activities including essay competitions, signing a non‐smoking pledge, Additional components: No‐Tobacco‐Day theme ...
But there is one key difference among the programs: Mr. Bloomberg's generosity is means-tested, given only to students whose family income is under $300,000 a year. The programs at Einstein and ...